How to Audit Your EHR Data Migration for Revenue Leakage?
A successful EHR data migration audit requires a three-way reconciliation between your legacy system's accounts receivable, your new platform's imported ledgers, and your clearinghouse's submission history.
Revenue leakage typically occurs when unworked denials or pending claims fail to map correctly to the new system, effectively freezing recoverable cash flow inside an inaccessible legacy archive.
The audit starts with a dollar-level comparison — not a file-count comparison. Most software vendors define a "successful" migration as data visibility. A practice owner defines it as money in the bank. Those are not the same measurement, and the gap between them is where recoverable revenue quietly disappears.
Three reconciliation streams surface that gap: the legacy AR report down to the claim level, the new platform's imported claim and patient balances, and the clearinghouse's record of what was actually submitted and acknowledged.
When the three don't line up, the mismatch is the leak — and every missing claim represents either a timely-filing deadline about to expire, a denial that should have been appealed, or a patient balance that was never carried over.
Migrations happen for good reasons — platform upgrades, cloud transitions, consolidation after a merger. None of those reasons change the structural financial risk that sits inside the transition itself.
Below is what the audit looks like in practice, where revenue tends to hide, and what to check before assuming your migration is actually complete.
- Why Your EHR Migration Demands Its Own Revenue Audit
- How to Audit an EHR Data Migration: The Three-Way Reconciliation
- Where Revenue Hides During an EHR Migration
- Who This Audit Process Is Not For
- Objections Practice Owners Raise About Migration Audits
- What Happens After the Audit: Closing the Leak Permanently
- Frequently Asked Questions
- Why does my AR report look different after migrating to a new EHR?
- What is the most common place for revenue to "hide" during a migration?
- Can a software vendor be held responsible for revenue leakage?
- How many months of legacy data should I audit?
- Does my clearinghouse data remain accurate during an EHR switch?
- How long does a post-migration audit typically take?
- What should I look for in a billing partner to handle the migration audit?
- The Bottom Line
Why Your EHR Migration Demands Its Own Revenue Audit
The vendor moved your data. Nobody automatically moved your money.
Two different events. Same day. Practices assume they're the same event. They aren't.
Most billing companies measure migration success by submission throughput. How fast data transferred. How many records mapped. Clean claims sail through. Complex ones quietly sit.
That's the volume-first model at its worst. Clean claims get paid. Complex claims get abandoned. And during a migration, everything complex is in motion at once.
A proper full-service chiropractic billing function verifies the money followed the data. A migration tool was never built to do that.
The Vendor's "Complete" and Yours Are Not the Same
When a vendor says "migration complete," they mean something specific. Every field that was supposed to map, did. Every record they contracted to transfer is visible in the new system.
That's a technical definition. Not a financial one.
Your definition is simpler. The money that was coming in last month is still coming in this month. Patient balances didn't evaporate. Denials that need appeals are in a queue somewhere. AR aging didn't reset because import timestamps got confused.
Two different definitions. Practice owners assume they overlap.
They don't.
The migration tool is a data transport system. It's not a reconciliation system. It moves records. It doesn't verify revenue. And most software contracts spell this out in writing — data-accuracy warranties rarely extend to financial continuity. The responsibility for proving your money followed your data sits with the practice, not the vendor.
Here's how the two definitions compare side by side:
| Definition aspect | Vendor's version of "complete" | Practice's version of "complete" |
|---|---|---|
| What counts as success | Records mapped, fields transferred, data visible in the new platform | Revenue collected after the switch matches revenue collected before it |
| Primary measurement | Claim-count completeness | Dollar-level reconciliation |
| Where liability ends | Data-accuracy warranty, usually capped at service cost | Financial continuity, sits with the practice |
| When the work ends | At the technical sign-off | After the audit confirms money followed data |
A few quick tells surface when the two definitions haven't lined up the way the vendor's dashboard suggests:
- Deposits running below expectations (the first financial signal — usually visible three to four weeks after go-live)
- Denials that previously required active appeals no longer appearing in any work queue in the new system
- Patient statements going out for balances that should have been offset by existing credits
- AR aging buckets that look cleaner than they should after a cutover (often a timestamp-reset artifact, not actual progress)
Same word. Two entirely different standards.
Why Most Practices Discover the Leak Three to Six Months Late
The volume approach handles the bulk of a migration cleanly. Straightforward coding, no modifier issues, standard claims. They import, submit, pay. That part usually looks fine.
Then a claim needs a medical necessity argument. Or a pending appeal. Or a documentation correction.
The automation model has nowhere to put it.
It doesn't fail loudly. It fails quietly. The claim migrates in a status the new system doesn't know how to read. Or it lands in an archive folder the new workflow never looks at.
So it sits. Then it ages. Then it dies.
Three months in, deposits start drifting below expectations. Six months in, aging AR reports surface a wave of claims that slipped past timely-filing windows. Twelve months in, untangling what happened is four times harder than catching it on day thirty.
EHR platforms marketed as billing solutions are where this gets worst. EHR software is a claim submission tool. Denial management, appeals, and AR recovery are judgment-driven functions. No platform automates them well. And a migration is exactly when those judgment-driven items quietly fall through the floor. The EHR Transition & Data Integrity Study has documented data loss and mapping errors as significant, under-acknowledged risks to financial continuity during platform transitions.
Most practices don't catch the leak during the migration.
They catch it during the audit that should have run alongside it — and that most never commissioned.
How to Audit an EHR Data Migration: The Three-Way Reconciliation
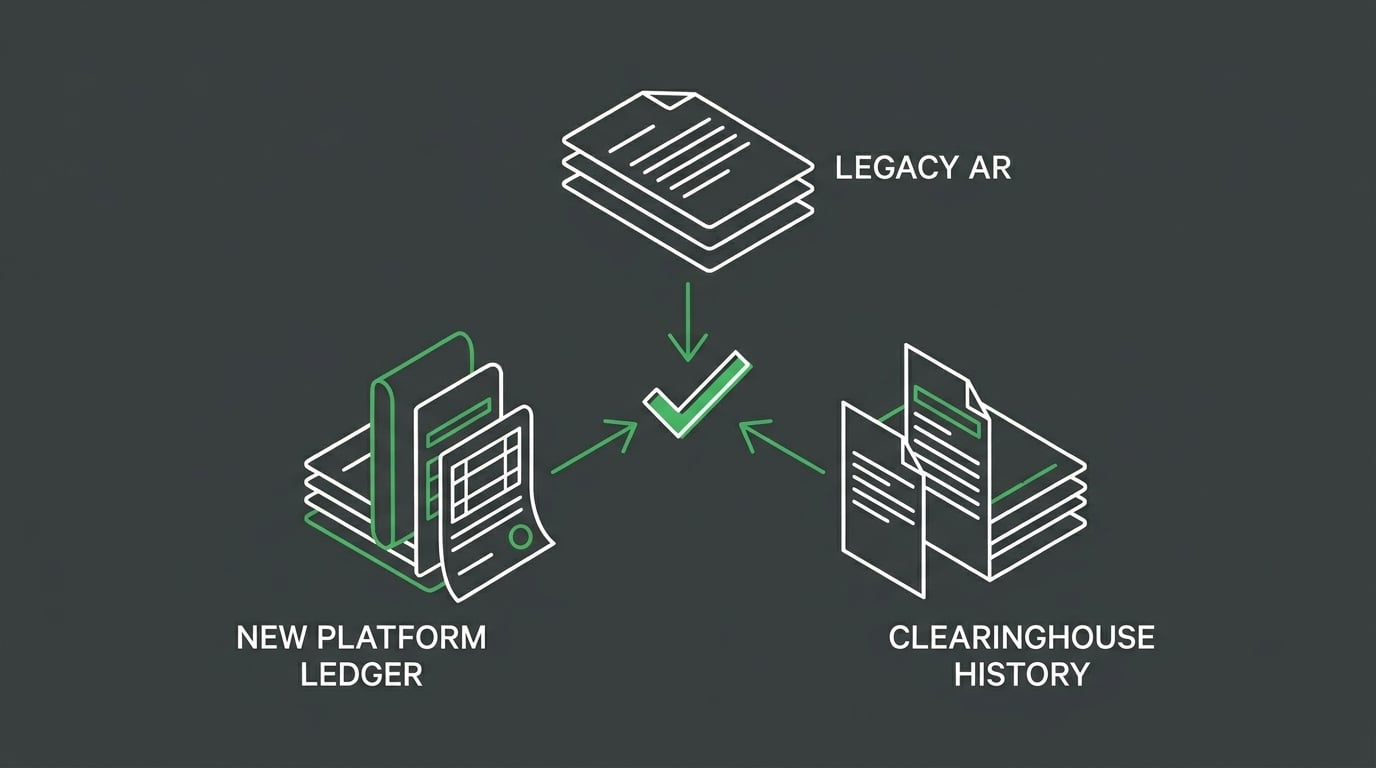
A migration audit isn't a dashboard review. It's a claim-level reconciliation between three independent sources of truth.
The question is simple. Does the money that existed in the legacy system match what the new system is tracking? Does the clearinghouse confirm both?
Three streams. One comparison.
The EHR Migration Risk Framework points to inadequate financial reconciliation between legacy and new systems as a core driver of post-implementation failure. Not software defects. Not field mapping errors. The absence of a structured financial check.
Each stream pulls from a different system and confirms a different piece of the picture:
| Reconciliation stream | Source of truth | What it confirms |
|---|---|---|
| Legacy AR export | Old EHR, pulled before decommission | Full claim-level financial snapshot at the migration moment |
| New platform ledger | New EHR, pulled after import | What the new system is actively tracking |
| Clearinghouse history | Independent third-party record | What was actually submitted, acknowledged, and paid |
When all three line up, the migration is financially complete. When they don't, every gap is a claim that needs to be worked, written off with documentation, or escalated.
Step 1: Export Your Legacy AR Down to the Claim Level
Before the legacy system is decommissioned, pull a complete AR export.
Not a summary. Not a dashboard screenshot. A claim-level export with every open charge, every aging bucket, every patient balance, every unapplied credit, and every claim status.
Four categories belong in that export that most operators forget:
- Denied claims — including the ones marked "closed" (these hold the appeal opportunities the new system won't surface on its own)
- Claims flagged as pending appeal — with the original appeal history attached to the record
- Patient responsibility balances — every open balance, not just the recently active ones
- Any claim with a note attached — those notes often contain the only record of why a claim was being worked manually in the first place
The goal is a static financial snapshot of your practice at the moment of migration.
If you can't produce that snapshot, you have no audit baseline. And the vendor's word becomes the only version of events.
Step 2: Pull the Imported Ledger From Your New Platform
On the other side of the migration, pull the matching export. Same fields. Same date range. Same level of detail.
This is where most practices find the first round of leakage.
Patient ledgers often import without the "unapplied credits" column. Aging buckets sometimes reset to the import date rather than the original claim date — which makes 120-day AR temporarily look like 30-day AR until the real aging catches up. Denied claims frequently import with a generic "closed" status that strips their appeal history.
MGMA Financial Management research on post-migration reconciliation identifies patient ledger reconciliation as the single most critical step in preventing post-migration AR aging.
It's also the step most commonly skipped.
Compare the two reports side by side. Line by line. Flag every claim where the status, balance, or aging doesn't match the legacy export.
Step 3: Cross-Reference Your Clearinghouse Submission History
Your clearinghouse is the third source of truth. It's the independent record of what was actually submitted, what was acknowledged, what was rejected at the payer level, and what was paid.
Pull clearinghouse submission data for the twelve to twenty-four months before the migration. Match every submitted claim against both the legacy export and the new platform's imported ledger.
Three kinds of discrepancies will surface:
- Claims the clearinghouse shows as submitted that don't appear in the new platform — the new system doesn't know to track them
- Claims the new platform shows as open that the clearinghouse shows as paid — payments posted against the wrong account, or not posted at all
- Claims denied at the clearinghouse level that never reached a denial work queue in either system — appeals that were never filed
The clearinghouse closes the loop. Without it, the audit only compares the two systems the migration touched. Both can be wrong in the same direction. Medical Billing Audit Standards treat regular claim-level auditing as one of the most reliable ways to surface revenue leakage caused by system-level transitions before it compounds.
Where Revenue Hides During an EHR Migration

The leaks are rarely dramatic. No single claim usually explains a ten percent cash flow dip.
It's the cumulative effect of small, structural mismatches the audit is built to surface. Some patterns repeat across almost every platform switch — and the ChiroTouch Cloud Specialists transition surfaces them especially cleanly.
Three categories show up more often than any others:
| Leakage point | How it hides | Financial symptom |
|---|---|---|
| Unworked denials | Migrate as "closed" or "archived" in the new system | Appeal windows pass quietly; denied revenue permanently lost |
| Unapplied credits | Credit fields fail to map field-to-field during import | Patients billed for balances that should have been offset |
| Documentation history | Supporting notes unlinked from claim records | Delayed audit defense failure; claim recoupments six to eighteen months later |
Each one is worth looking at in detail.
Unworked Denials That Migrated as "Closed" or "Archived"
This is the biggest category. By a lot.
In the legacy system, a denied claim sits in a work queue. It waits to be appealed, written off, or overturned. In the new system, that same claim often imports with its denial history compressed into a status code the new platform doesn't flag for action.
It reads as "closed." Nobody touches it. No alert fires. The appeal deadline passes.
The audit catches these by cross-referencing denial-reason codes from the clearinghouse against open status fields in the new platform. Any claim denied but not currently in an active work queue is a candidate for recovery — as long as the payer's timely-appeal window hasn't closed yet.
Unapplied Credits and Orphaned Patient Balances
When patient accounts migrate, the unapplied-credits bucket is one of the most likely things to fail mapping.
Three categories of credits are especially vulnerable during a platform switch:
- Previous patient overpayments — historical surplus payments sitting on file
- Pre-paid visit packages — balance remaining on package deals purchased before the migration
- Insurance overpayments awaiting adjustment — payer-side surpluses that still need to be refunded or offset
These ledger items rarely have a clean field-to-field match across platforms. When they don't import, two problems follow.
Patients get billed for balances that should have been offset by existing credits. That damages the clinical relationship. And the practice loses visibility into liabilities it still technically owes.
The audit pulls the legacy unapplied-credit register and reconciles it against any patient-level credit field in the new system. Every credit that doesn't appear needs to be manually re-applied.
Before a patient calls to ask why.
Medical Necessity Documentation That Didn't Transfer
This one doesn't cause an immediate cash flow problem. It causes a delayed audit defense problem.
Chiropractic billing depends heavily on documentation history. AT modifier justifications. Active versus maintenance care determinations. Plan of care notes tied to specific claim dates.
When a migration moves claim data but flattens or omits the linked documentation, the evidentiary trail breaks.
Six to eighteen months later, a payer audits a batch of claims. The supporting documentation is either inaccessible in the legacy system or missing from the new one. The claim gets recouped. The practice pays money back.
The root cause traces to a migration that looked complete on day one.
That's part of why ChiroTouch Cloud Specialists factor the full cost of platform transitions well beyond the immediate cash flow dip — documentation risk is a months-later exposure that the original audit is the only place to catch.
Who This Audit Process Is Not For
An audit is work. Not a dashboard glance.
The practices that get the most out of one are the ones willing to engage with what it surfaces. Two buyer behaviors usually drop out at this stage. Neither is wrong. They just aren't a fit for the work.
If Rate Is the Only Filter
If the first and only question is "what does this cost?" — this probably isn't the right conversation.
Not because the question is wrong. Because the answer doesn't tell you anything useful about whether the audit recovers what it's supposed to. A few things actually do:
- Scope — how many months of claims, how many sources of truth the reconciliation pulls from
- Reconciliation methodology — whether all three streams get compared, or just the two the migration touched
- Denial-recovery work on the back end — what happens to claims the audit surfaces as still-appealable
Those determine outcomes. Rate determines cost. Two different conversations.
Price competition drives volume models. Volume models deprioritize high-friction, high-value claims. A migration audit is the definition of high-friction, high-value work. Scope it to the cheapest version possible, and the leaks that matter most are exactly the ones it will miss.
If rate is the decision, this isn't the right call.
If You Want to Stay Out of the Reconciliation Itself
Effective reconciliation is a working partnership. Not a hands-off handoff.
Three things need active practice involvement:
- Pulling the legacy export before the old system gets decommissioned — once the legacy platform is offline, that snapshot is unrecoverable
- Providing context on claims that were being worked manually — no system documents why a claim is in someone's work queue
- Confirming which patient-balance credits were legitimate versus artifacts of older software quirks — only the practice knows which credits are real
If the expectation is zero engagement — no EHR access, no documentation cooperation, no provider availability for appeal clarifications — the audit's results will be correspondingly thin.
Some of the most valuable claims will stay unrecoverable. Not because they're objectively dead. Because nobody inside the practice can corroborate the history the audit needs to rebuild them.
Objections Practice Owners Raise About Migration Audits

Most practice owners don't resist the idea of an audit. They resist the framing that it's separately necessary after a migration the vendor has already called complete.
Two questions come up almost every time.
"The Software Vendor Said the Migration Was Complete."
It probably is. By the vendor's definition.
The vendor's definition: records mapped, fields transferred, the new system displays what the old system held. That's a data migration.
It's not a revenue migration.
Submission is not billing. Getting paid is billing. The gap between "records are visible" and "money is being collected correctly" is where the vendor's responsibility ends and the practice's starts. Software contracts usually spell this out in writing. Data-accuracy warranties rarely extend to financial continuity.
The vendor isn't wrong to declare their piece complete. The audit isn't a rebuke of the vendor. It's the financial companion to the technical handoff.
And it belongs to the practice, not the software company.
"Our Clearinghouse Has All the Data We Need."
It has all the submission data you need. It doesn't have all the billing data.
The clearinghouse can tell you what was sent. What was paid. That's the whole list.
It can't tell you any of the things that actually matter after a migration:
- Which claims were denied for a medical-necessity reason and are still appealable — denial reason codes live at the clearinghouse, but the workable status lives in the EHR
- Whether a patient balance was offset by a pre-existing credit — the clearinghouse never sees patient-level ledger activity
- Whether the new platform's aging buckets correctly reflect the original claim dates — aging is a function of the EHR's timestamp handling, not the clearinghouse's
The clearinghouse is a critical leg of the audit. It isn't the whole audit.
Treat it as a single source of truth and you miss exactly the leaks a migration causes — the ones that live in the space between systems, not inside any one of them.
What Happens After the Audit: Closing the Leak Permanently
An audit without follow-through is a report that gets filed. The leaks get documented. Then they re-open, because the conditions that created them didn't change.
Verifying billing software compatibility after a migration is part of the fix. The larger change is structural, not technical. Two habits the migration period exposes, and that the ongoing work depends on:
- A weekly communication cadence — not a monthly summary, not a quarterly review
- A structural audit rhythm — quarterly or twice-yearly, not once-and-done after a crisis
Both below.
Establish a Weekly Communication Cadence
Silence from a billing function isn't professionalism. It's a structure that hides problems until they become cash flow crises.
The migration period is the most extreme version of that risk. The same dynamic operates in steady state.
Without a weekly touchpoint — claims submitted, claims paid, denials worked, AR trending — problems surface at month-end or quarter-end. By then, the workable window on most of them has already closed.
A weekly cadence doesn't add labor. It redistributes work that was already happening and makes the outputs visible.
You see what's working. The biller surfaces what's stuck. And the migration-era blind spots stop repeating.
Make the Audit a Structural Check, Not a One-Time Rescue
The strongest version of this work isn't a single post-migration audit. It's a review cadence. Quarterly, or at a minimum twice a year. Catching small leaks before they compound.
That's what active revenue defense actually looks like on a week-to-week basis.
Not a dashboard glance. Not a year-end reconciliation. A continuous working review of what's being submitted, what's being denied, what's being appealed, and what's aging.
The audit is the first instance.
The cadence is the solution.
Frequently Asked Questions
Why does my AR report look different after migrating to a new EHR?
Mapping logic often groups aged claims differently or fails to import unapplied credits, creating a false impression of your practice's financial health. The numbers aren't necessarily wrong from the new system's perspective — they just don't reflect the financial reality of the legacy system at the moment of cutover.
Aging buckets are especially prone to distortion. Some systems reset timestamps to the import date instead of the original claim date. That makes 120-day AR temporarily look like 30-day AR until the real aging catches up. The report isn't lying. It's just telling you a different story than the one your bank balance is telling you.
What is the most common place for revenue to "hide" during a migration?
Unworked denials in the legacy system often migrate as "closed" or "archived" files, preventing the new system from alerting you to the need for an appeal. They're still technically visible. Just not actively surfaced for work.
Because no alert fires, no one looks. The claim sits. The appeal window passes. The revenue is effectively gone — even though the claim itself is still right there in the new platform, readable at any time. That's the quiet part of the problem. Nothing disappeared. Nothing got flagged either.
Can a software vendor be held responsible for revenue leakage?
Most software contracts have limited liability clauses regarding data migration accuracy, and the vendor's liability is usually capped at the cost of the service — not the downstream financial impact of mapping errors. That's a contractual reality, not a judgment on the vendor.
So the burden of financial reconciliation sits with the practice. The audit is how that burden gets discharged — by independently verifying the revenue followed the data, rather than treating the vendor's technical sign-off as a financial one. Two different sign-offs. Only one of them pays the bills.
How many months of legacy data should I audit?
At a minimum, audit the last 12 to 24 months of AR. That range covers the timely-filing window for most payers and ensures recent denials haven't slipped past their appeal deadlines unnoticed.
For practices with significant personal injury (PI) liens or long-running patient balances, extend the window further. PI claims can stay open for years. A migration is one of the most common points at which those claims quietly disappear from view — and once they do, they're unlikely to resurface without a deliberate search.
Does my clearinghouse data remain accurate during an EHR switch?
Yes. The clearinghouse operates independently of the practice's EHR, so it keeps its own record of what was submitted and what was paid regardless of which platform the practice migrated to or from. That's exactly why it's useful as a third reconciliation stream.
But it has to be cross-referenced with the new EHR to verify the loop is closed on each claim. Payments posted. Denials routed. No claims stranded between systems. The clearinghouse tells you what went out and what came back. The EHR is where you confirm what happened after that.
How long does a post-migration audit typically take?
Duration varies with the volume of legacy claims and the complexity of the denial history. A straightforward practice with clean records can complete a three-way reconciliation in a matter of weeks.
A practice with significant unworked AR, PI lien exposure, or documentation gaps takes longer. The earlier the audit starts, the shorter it tends to run — and the more recoverable revenue it typically surfaces. Wait six or twelve months after the migration, and a meaningful percentage of the leakage has already aged past the point of recovery.
What should I look for in a billing partner to handle the migration audit?
Three things are worth evaluating before the rate conversation even starts:
- Specialty expertise — chiropractic documentation standards, AT modifier rules, PI workflows are not universal billing skills
- A reconciliation methodology that pulls from all three sources of truth — not just the new EHR
- Proactive communication — weekly updates on what's been found, what's been recovered, and what's still open
A partner that treats the audit as a one-time transaction misses the point. The audit surfaces the problem. The structural cadence afterward is what keeps it closed. Platform-specific insights from resources like ChiroTouch Cloud Specialists help surface the mapping issues that show up as part of that ongoing process.
The Bottom Line
The question isn't whether your EHR data migration is complete. The vendor has already told you it is.
The question is whether your revenue is still intact.
The vendor's definition of "complete" doesn't answer that. It was never built to. A migration moves data. It doesn't verify that the money being collected before the switch is still being collected after it.
Submission is not billing. Getting paid is billing.
Practices that come out of a migration with their revenue intact are the ones that ran the audit separately. Not because they distrusted the vendor. Because they understood the two definitions of success don't meet in the middle.
Those aren't the same thing.
Migrations move data. They don't verify the revenue behind that data actually made the trip.
A practice assessment walks through the three-way reconciliation — legacy AR, new platform ledger, clearinghouse history — and surfaces what's recoverable, what's stranded, and what's quietly aging past the appeal window while the new system reports everything as fine.
Book a Call to see what didn't migrate with your data.
The vendor's definition of "complete" and your bank deposits are two different numbers. The audit is how you find out which one is telling the truth.
© 2026 Bushido Billing. All Rights Reserved | Web Design by iTech Valet


