Why is the ChiroTouch Cloud Migration Causing Billing Interruptions in 2026?
ChiroTouch Cloud migrations are interrupting billing in 2026 because moving from a local server to the Cloud doesn't simply relocate your data — it shifts your practice into a different security architecture that your clearinghouse credentials were never configured for.
When the on-premise server comes down, Trading Partner IDs, NPI mappings, ERA associations, and API tokens don't always travel cleanly across the handoff. The result is claims that look submitted inside your ledger but never reach the clearinghouse, ERAs that stop auto-posting, and batch transmissions that stall behind new multi-factor authentication prompts nobody planned to handle manually.
This isn't a software bug. It's a credentialing and mapping gap between ChiroTouch Advanced (or Core) and your downstream partners at TriZetto and Change Healthcare.
Most of the damage happens quietly, in the Accounting module, where claims show "Ready to Submit" but never move. Practices usually catch on when AR starts aging with no posted denials and no clearinghouse rejections to explain the silence.
Fixing the interruption is forensic work on each broken credential — not a software patch and not a support ticket. Trading Partner IDs need re-verification. NPI mappings need to be rebuilt. API tokens need OAuth 2.0 re-authentication. MFA settings need configuration for automated batch workflows, or the claims won't send on schedule.
Below, we walk through exactly what breaks during the migration, why it breaks, how to identify the invisible AR that builds up, and what a proper post-migration audit looks like — so your cash flow comes back online with the software, not weeks after it.
Last Updated: April 20, 2026
- What's Actually Breaking When ChiroTouch Moves to the Cloud
- Why Most Responses to the Migration Fail
- The Five Credential and Security Breakpoints
- The Invisible AR Problem After Go-Live
- What a Post-Migration Audit Actually Looks Like
- Frequently Asked Questions
- Why are my ChiroTouch claims "Pending Submission" for weeks?
- How do I fix the NPI mismatch error?
- Why are my ERA files not posting automatically?
- Do I need new TriZetto login credentials?
- How do I re-verify my Medicare Provider ID?
- Can I revert back to ChiroTouch Server?
- Should I just wait for a ChiroTouch software fix?
- The Migration Is a Credentialing Project, Not a Software Update
What's Actually Breaking When ChiroTouch Moves to the Cloud
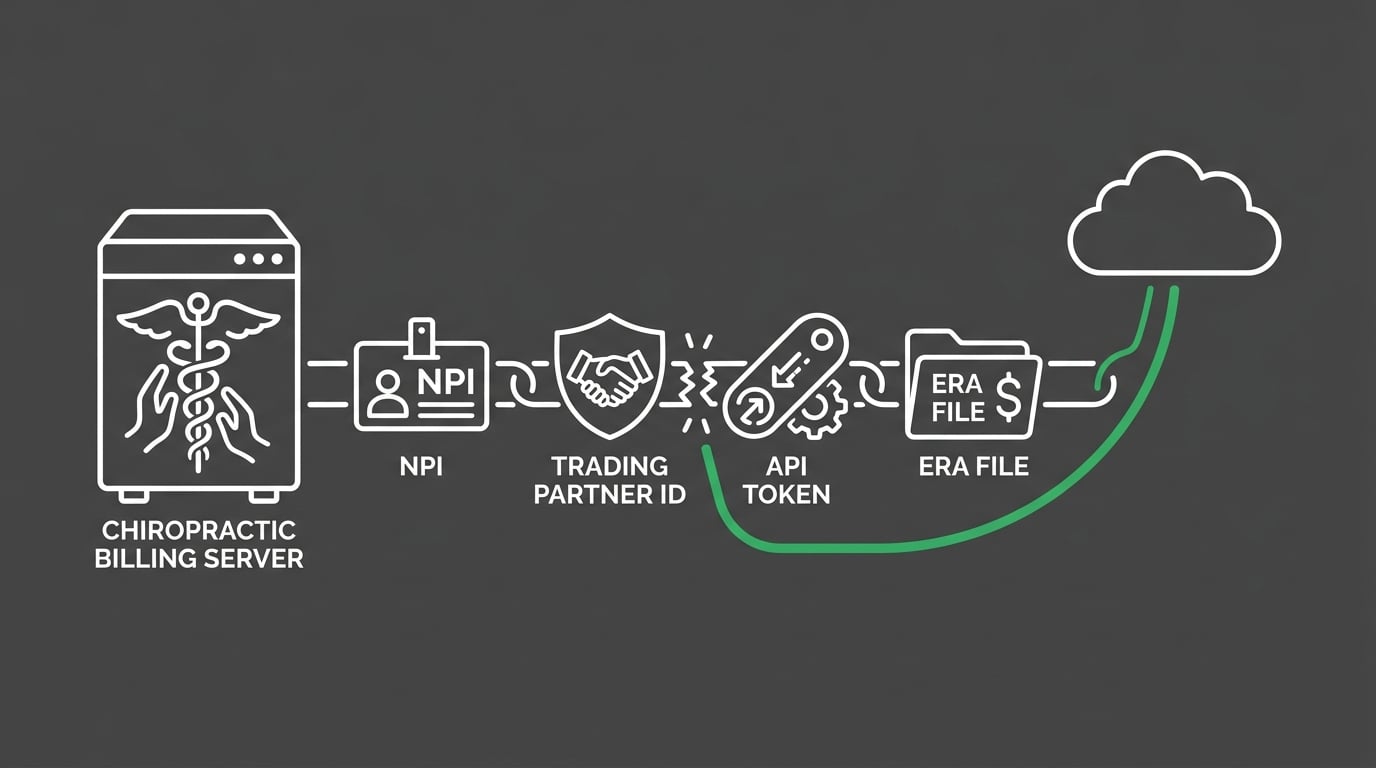
A Cloud migration isn't a software upgrade. It's a credential reset dressed up as one.
That distinction decides everything that happens next. Practices that plan for a software event plan for installation, training, and login changes. Then the full-service chiropractic billing operation that ran cleanly on the old Server install stops producing collections three weeks after go-live, and nobody inside the clinic can explain why.
The reason is mechanical. Every claim your practice sends depends on a chain of identifiers that have to transfer cleanly into the new environment. On Server, those identifiers lived in flat configuration files ChiroTouch read directly. In the Cloud, they live inside a managed identity layer that talks to your clearinghouse through a completely different protocol.
The software moved. The credentials didn't — at least not cleanly, and usually not completely.
Six specific identifier types get disrupted in almost every Cloud migration:
- NPI (National Provider Identifier) — The field that tells payers which provider rendered the service. Migration can reset this in the Accounting module to stale or default values, which produces silent rejections at the clearinghouse edge.
- Tax ID (EIN or SSN) — Attached to practice-level enrollment. A mismatch between ChiroTouch and the clearinghouse breaks electronic submission at the account level, not the claim level.
- Trading Partner ID (TPID) — The identifier TriZetto or Change Healthcare uses to route your submissions. Frequently reset to a default value when the accounting database migrates, which is one of the most common silent failures.
- Payer Sub-IDs (enrollment ID per payer) — Each payer assigns its own enrollment number. Migration sometimes drops these entirely, which breaks both claim submission and ERA reassociation for that specific payer.
- API Tokens (OAuth 2.0 credentials) — The machine-to-machine authentication between ChiroTouch Cloud and the clearinghouse. Tokens expire, get regenerated, then sit unapproved on the clearinghouse side until someone asks them to approve.
- ERA Enrollment Mapping (sub-ID linkage) — Connects remittance files back to the original claims. Corruption here produces ERAs that arrive but don't post, or post to the wrong claim entirely.
Most of the billing interruptions practices see in the first thirty days trace back to at least two of those six. Not to ChiroTouch the product. Not to TriZetto the clearinghouse. To mapping work that never got scoped — because the migration was sold as an update instead of what it actually is.
The Assumption That Sinks Most Migrations
Most practices plan the migration as a day-of event. That's the mistake.
A day-of plan covers what happens the day the software switches. It doesn't cover what happens the next morning when the first batch of claims sits in "Pending Submission" and nobody knows why. Or the week after, when the first ERA file doesn't auto-post and the accounting ledger starts drifting out of sync with reality.
Silence in a billing pipeline isn't professionalism. It's a structural problem that hides revenue loss until the loss stops being recoverable.
If the migration plan didn't include a credential audit before go-live and a reconciliation pass in the first two weeks after, it wasn't a migration plan. It was an install checklist.
Why "Ready to Submit" Doesn't Mean "Received"
This is where most practices get fooled by their own software.
ChiroTouch's ledger tracks local status. A claim marked "Ready to Submit" means the software packaged the claim correctly. That's the entire meaning of the status. It says nothing about whether the clearinghouse accepted the claim, whether the API handshake worked, or whether the claim ever left the Cloud instance at all.
On Server, a failed transmission usually threw a visible error. On Cloud, failed transmissions increasingly fail quietly at the authentication layer. The claim holds steady in "Ready" status while the API request gets refused upstream at TriZetto or Change Healthcare.
You don't see the rejection inside ChiroTouch. You see it thirty days later, in an aged AR report with no posted response and no rejection code to explain the silence.
This exact pattern is documented in the ChiroTouch Advanced Release Notes for Q1 2026, which address the "Sync Error 401" that migrated accounting ledgers commonly produce when API credentials haven't been re-authenticated against the new Cloud handshake. The software isn't lying to you. It's just not in a position to know.
Why Most Responses to the Migration Fail
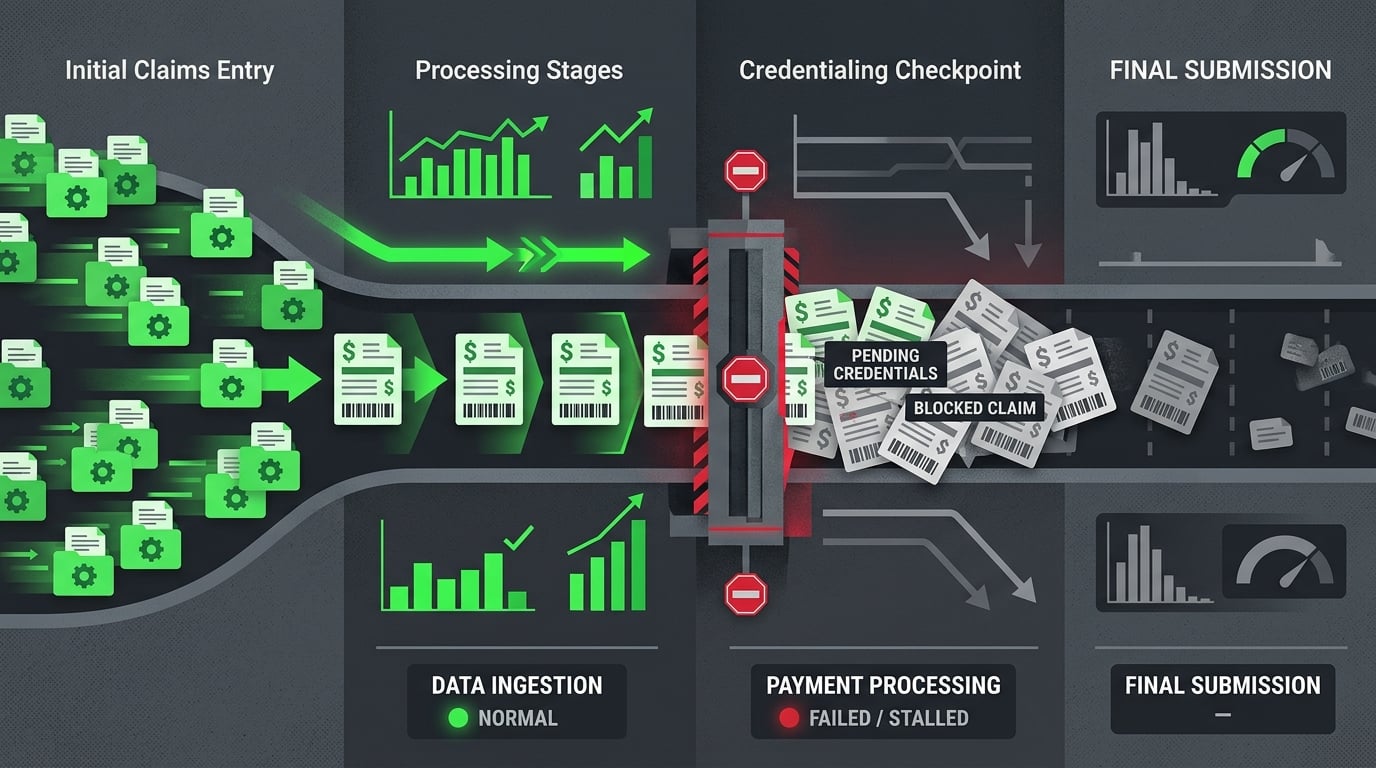
The default response to migration billing problems always looks the same. Call support. Open a ticket. Tell the billing team to keep submitting and see what clears. Wait for the vendor to push a fix.
None of that resolves the underlying issue, because the underlying issue isn't in the software.
It's in the credentialing layer — the handshake between ChiroTouch and your clearinghouse, and between your clearinghouse and each of your payers. Treat it as a software problem and the clock burns for six weeks while nobody's actually working on the fix. By then, the earliest stalled claims are already aging past the point of clean recovery.
The post-migration timeline runs on its own clock whether anyone is watching it or not:
- Week 1 (Go-Live) — Everything looks normal. Claims enter the system. The ledger balances. No visible errors appear. This is the most dangerous week because the assumption that "things are fine" gets baked in before anything's been verified.
- Weeks 2–3 (Silence Begins) — ERAs stop posting. Rejections don't appear. Denials aren't routing. The billing team sees a quiet week and attributes it to the migration settling in.
- Weeks 4–5 (Pattern Emerges) — AR starts aging with no movement. The first inquiries about unpaid claims come in. Someone finally notices the clearinghouse portal shows no record of claims ChiroTouch says were sent.
- Week 6+ (Recovery Window Narrowing) — Commercial payers with 90-day windows are burning their clock. Medicare still has runway but needs fast identification. Recovery shifts from cleanup to triage.
Why the Volume-First Billing Model Breaks Under a Migration
Most billing operations run on throughput. Submit volume. Post ERAs. Work denials that auto-route themselves. Move to the next batch. That's the model.
The model works when the pipeline is clean. It falls apart the moment the pipeline gets interrupted — and a migration interrupts the pipeline in ways the dashboard doesn't display.
Here's how it actually unfolds. Claims stop moving. ERAs stop posting. Denials stop appearing. A throughput operation sees a quiet week and assumes things are fine.
By week three, the problem is visible. By week five, the earliest stalled claims are pushing into timely filing windows for commercial payers.
The volume model has no diagnostic step built into its workflow. It doesn't check whether the pipeline still exists, because its entire design presumes it does. When the migration hands you a broken pipeline, nobody inside a volume operation is structurally responsible for catching it.
That's not a staffing issue. It's a model issue. It's the same model issue that keeps practices stuck in survival billing instead of securing predictable clinic cash flow — and the migration just exposes the gap faster than usual.
It's also why a human biller becomes necessary to fix ChiroTouch Cloud migration errors. No automated routing catches a claim that never transmitted. Someone has to look.
The Cost of Waiting for a "Software Fix"
Here's the honest part. ChiroTouch's support team can resolve problems inside the application. They can't fix your clearinghouse enrollment. They can't reset your Trading Partner ID at TriZetto. They can't re-enroll your ERAs with each payer. They can't re-authenticate your API tokens on your behalf.
All of that work lives outside their building. Waiting for them to solve it is waiting for something that was never going to happen.
Meanwhile, the clock keeps running. Medicare's one-year timely filing window doesn't pause for migrations. Most commercial payers run 90 to 180 days. State Medicaid programs run anywhere from 60 to 365 days, depending on the state.
Every week credentialing waits is a week of claims aging into harder territory. Some of them — especially Medicare, Medicaid, and certain state-regulated plans — won't come back once they cross the window.
Waiting is expensive. Diagnosing is cheap. Most practices do them in the wrong order.
| Migration Response | What It Addresses | What It Misses | Revenue Impact |
|---|---|---|---|
| Call ChiroTouch Support | Software bugs inside the application | Clearinghouse credentials, API tokens, ERA enrollment, payer-level IDs | High — clock keeps running on stalled claims |
| Submit more claims anyway | Maintains data entry momentum | The entire transmission layer is broken; new claims stall behind old ones | High — compounds invisible AR |
| Wait for the "next update" | Assumes vendor can fix downstream issues | Most credentialing fixes happen outside ChiroTouch entirely | High — timely filing windows expire during the wait |
| Audit every credential at the protocol level | Actually resolves the root cause | Requires expertise in ChiroTouch, TriZetto, and payer enrollment simultaneously | Low — claims resume once credentials are rebuilt |
The Five Credential and Security Breakpoints

Most migration interruptions trace back to one of five specific breakpoints. They aren't random failures. They follow a predictable pattern tied to how ChiroTouch's Cloud architecture handles credentials differently than the Server version handled them.
Knowing which breakpoint is active in your instance is the difference between a three-day recovery and a three-month one. All five can fail at once. Usually at least two of them do.
Five telltale symptoms usually point to which breakpoint is active:
- Claims stuck in "Submitted" status with no clearinghouse record — Usually points to NPI or Trading Partner ID desync at the clearinghouse edge, where the credential doesn't match what the clearinghouse has on file.
- Claims stuck in "Pending Submission" for weeks — Points to OAuth 2.0 token re-authentication that didn't complete, or did complete but never got approved on the clearinghouse side.
- Overnight batch jobs that used to run silently now time out — Points to MFA enforcement blocking the automated transmission script because no human is present to answer the authentication prompt.
- ERAs visible in the clearinghouse portal but not posting inside ChiroTouch — Points to ERA reassociation sub-ID corruption in the mapping layer between clearinghouse and Cloud instance.
- Medicare claims rejected or disappearing entirely — Points to MBI mapping reset at the CMS interface layer, often combined with broken rejection routing that hides the problem from the biller.
NPI and Trading Partner ID Desync in the Accounting Module
Inside the Accounting application, there's a section called Maintain Trading Partners. It holds the identifiers that tell your clearinghouse which practice and which provider owns each claim.
During migration, those fields often reset to defaults or pull stale data from old configuration files. An NPI that doesn't match what TriZetto or Change Healthcare has on file produces a silent rejection at the clearinghouse edge. The claim never reaches the payer.
ChiroTouch still shows the claim as submitted. The clearinghouse has no record of it. Nobody finds out until somebody goes looking.
The fix is side-by-side work. Every Trading Partner ID inside ChiroTouch has to be checked against current clearinghouse records. Wherever they don't match, the practice has to re-register the connection. There's no shortcut.
OAuth 2.0 and API Key Re-Authentication
Pre-Cloud, ChiroTouch talked to clearinghouses over SFTP connections with static credentials. Post-Cloud, those connections move to OAuth 2.0 — a different handshake protocol with different rules.
The TriZetto Provider Solutions 2026 Cloud API specification requires every practice to re-authenticate its API tokens through the new flow before automated transmissions can resume. If your OAuth tokens weren't regenerated during the migration window, or were regenerated but never approved on TriZetto's side, nothing transmits.
It doesn't matter how clean the claim is inside ChiroTouch. The clearinghouse has never authorized the connection to receive it.
This is one of the single most common causes of claims stuck in "Pending Submission" for weeks after go-live. Your software holds the claim. Your clearinghouse doesn't know your software exists yet.
MFA Mandates Breaking Automated Batch Transmissions
The HHS Security Rule updates finalized for 2026 require multi-factor authentication for all Cloud-based ePHI access. ChiroTouch's Cloud environment enforces this at the session level, which is appropriate for user logins.
The problem shows up somewhere else. Automated batch transmissions — the overnight scripts that send claims, pull ERAs, and post remittances — don't have a human present to answer an MFA prompt.
In practice, batch jobs that ran flawlessly on Server can stall silently on Cloud. The submission script fires. It hits the MFA gate. It waits for input that never comes. It times out, often without logging anything useful.
The fix means configuring service accounts with the right authentication scope — enough to satisfy HHS, not so much that it blocks automated workflows. It's a specific configuration task, not a toggle in the main UI.
ERA Reassociation Failures
Electronic Remittance Advice files rely on sub-IDs that connect each remittance back to the original claim and to your practice's enrollment at each payer. Migration frequently drops or resets those sub-IDs in the mapping layer.
The symptom is ERAs that show up in your clearinghouse portal but don't auto-post into ChiroTouch. Or worse, ERAs that post to the wrong claim because the mapping is partially intact and partially corrupted.
Rebuilding this requires working with your clearinghouse to re-verify enrollment sub-IDs and re-map them inside the Cloud instance. It's not a one-click process, and it's not work anyone's going to volunteer for on your behalf.
Medicare Beneficiary Identifier Mapping Resets
Medicare claims depend on the Medicare Beneficiary Identifier format and the PTAN registration state. Migration sometimes resets how ChiroTouch stores and transmits the MBI — especially for practices that had custom validation rules on their Server install.
The effect: a Medicare claim that passes ChiroTouch's internal validation but gets rejected at the CMS edge for a malformed or outdated identifier. Rejections may route back through the clearinghouse cleanly. They may also disappear into "not submitted" status, depending on where the protocol broke.
Given the CMS MLN interoperability standards governing how Medicare data moves through EHR systems, a practice that skips MBI mapping verification after migration isn't just risking collection delays. It's sitting on information-blocking exposure, too.
| Breakpoint | Where It Lives | Typical Symptom | Fix Owner |
|---|---|---|---|
| NPI / Trading Partner ID Desync | Accounting > Maintain Trading Partners | Claims stuck in "Submitted" with no clearinghouse record | Clearinghouse + Practice |
| OAuth 2.0 / API Re-Auth | ChiroTouch Cloud API layer + TriZetto portal | "Pending Submission" persists for weeks | Clearinghouse + ChiroTouch admin |
| MFA Blocking Automation | Cloud security layer | Batch jobs silently time out overnight | Cloud admin + billing operations |
| ERA Reassociation Failure | Enrollment sub-ID mapping | ERAs in clearinghouse portal but not auto-posting | Clearinghouse + Practice |
| MBI Mapping Reset | Medicare-specific validation rules | Medicare claims rejected or missing | Clearinghouse + Practice + CMS |
The Invisible AR Problem After Go-Live
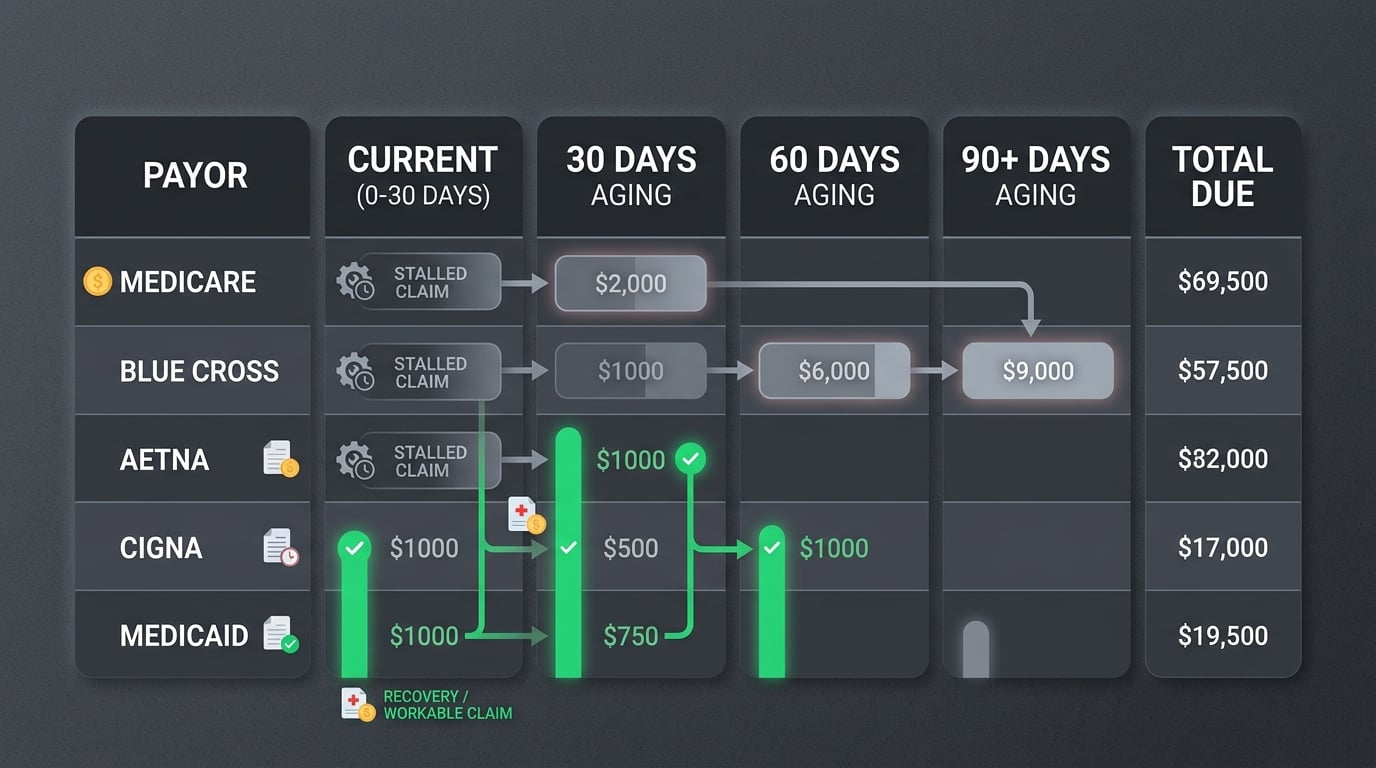
The most expensive part of a failed migration isn't the technical error itself. It's the gap between when the failure starts and when anyone inside the practice realizes it has.
Invisible AR is the name for claims that exist, look submitted, and never reach anybody. They age. They don't produce denials. They don't produce ERAs. They don't produce collections. They just sit there — costing the practice nothing visible, and everything eventually.
This is the category of damage that recovering lost claims data after a ChiroTouch server-to-cloud switch is specifically built to address. The ledger can't tell you what's missing from it, because from the ledger's perspective, nothing is.
Invisible AR shows up in a few specific ways across the ledger:
- "Pending Submission" claims with no clearinghouse confirmation — The software thinks the claim is queued. The clearinghouse has no record of it. Reconciliation against submission logs is what exposes the gap.
- Claims marked "Submitted" with no corresponding 999 or 277 acknowledgment — Submission shows on the ChiroTouch side, but no clearinghouse acceptance or rejection came back. The claim never actually cleared the authentication layer.
- Open balances on claims that were actually paid pre-migration — Payment came through, but the ERA mapping dropped, so the remittance never posted. AR reports show the claim open when the money arrived weeks ago.
- Posted ERAs attached to the wrong claim — Partial ERA mapping corruption routes a payment to a claim it doesn't belong to. Both the correctly-paid claim and the mis-posted claim end up showing false balances.
- Claims with "Ready" status for 30+ days — A claim that hasn't moved from "Ready" in a month isn't queued. It's stalled. The system isn't going to process it without someone stepping in.
How Claims Get Stuck in "Pending Submission"
Inside ChiroTouch, "Pending Submission" looks like a claim about to transmit. Post-migration, it often means a claim that's been waiting on an authentication handshake for weeks.
The front-end doesn't distinguish between "awaiting next batch" and "stuck behind a broken API token." Both states display identically. A biller scanning the claims list sees normal status while the transmission layer stays silent.
A real post-migration audit reconciles ChiroTouch's internal status against clearinghouse-side submission logs. Any claim marked Pending in ChiroTouch with no corresponding log entry at the clearinghouse is stalled — regardless of what the status field says.
The status field is just a field. It isn't proof of anything.
Why Aged Pre-Migration Claims Need Their Own Recovery Path
Claims submitted in the final two weeks before migration are often the most exposed. They may have been accepted at the clearinghouse but not yet paid when the cutover happened.
When the ERA comes back — assuming the reassociation layer is broken — the remittance doesn't post to the pre-migration claim correctly. The practice ends up with paid claims that still show open balances, and open claims that may have already been paid but aren't reflected anywhere in the Cloud ledger.
Cleaning that up takes manual reconciliation between the clearinghouse's remittance history and the new ledger. The software doesn't do this work automatically, and most billing operations aren't staffed to handle it as a batch project on top of current-week submissions.
The Timely Filing Clock That Doesn't Care About the Migration
Timely filing windows don't pause for software transitions. Medicare runs a one-year window from date of service. Most commercial payers run 90 to 180 days. State Medicaid programs range from 60 to 365 days, depending on state.
A claim stuck in "Pending Submission" for six weeks burns 60 days of a 90-day commercial window before anyone at the practice notices. By the time an audit runs, some of those claims are already past recovery — not because the service wasn't rendered, but because the submission technically never happened inside the window.
This is where migration interruptions quietly become permanent losses. And it's the single biggest reason most practices underestimate what's at stake when they treat this as a software issue instead of a process one.
What a Post-Migration Audit Actually Looks Like
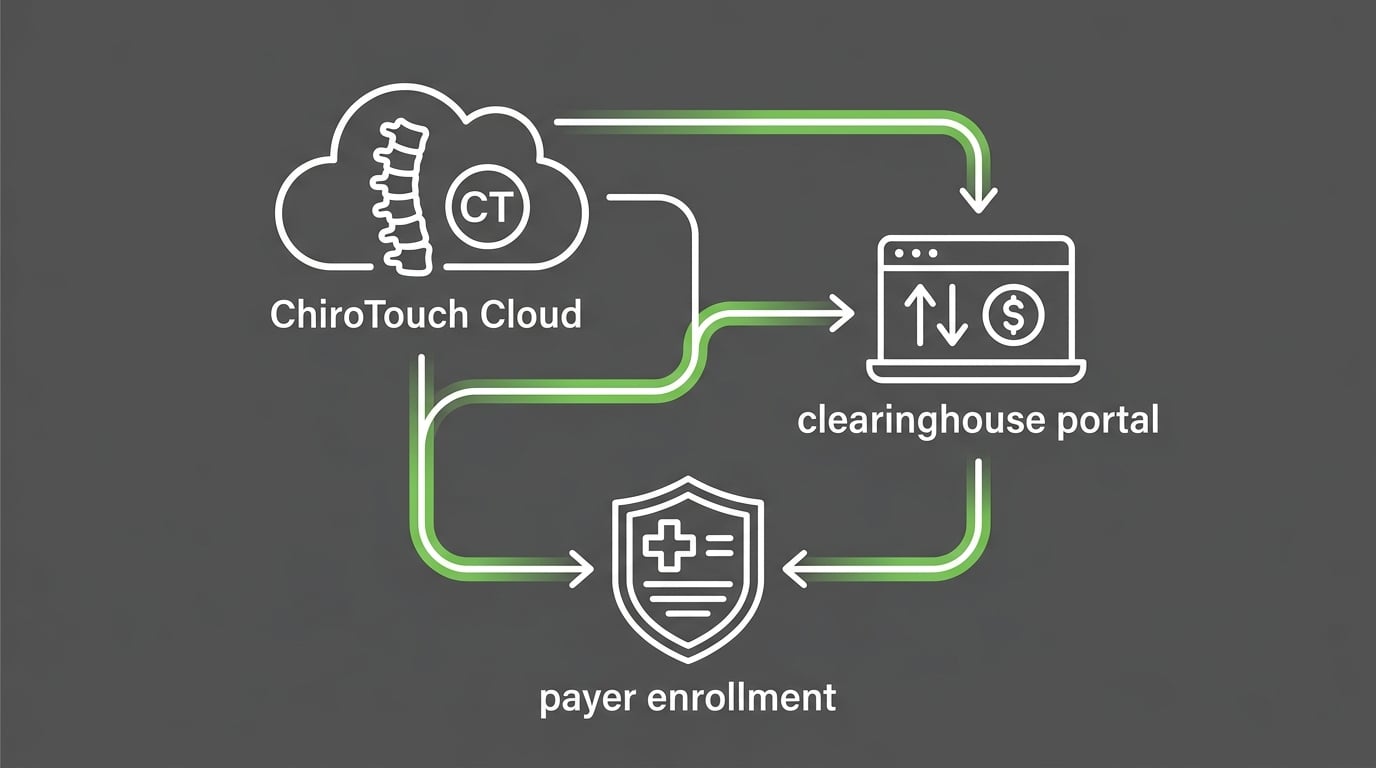
A real post-migration audit isn't a checklist someone runs inside ChiroTouch. It's a reconciliation project that spans the software, the clearinghouse, every payer enrollment, and the practice's own administrative records.
The work is technical. It's specific. It sits outside the scope of normal billing throughput. And it has to be done by someone who operates across all three environments — not someone who only operates inside one of them.
Who Should Actually Be Running the Audit
Reconciling ChiroTouch Cloud to TriZetto to individual payers is a three-system problem. Anyone working inside only one of those systems is going to miss breakpoints in the other two.
The work requires:
- Direct ChiroTouch Cloud admin access — to verify Trading Partner IDs, NPI fields, API token state, and ERA mappings inside the Accounting module.
- Clearinghouse portal access at TriZetto, Change Healthcare, or whichever partner your practice uses — to confirm credentials register correctly on their side, and that submission logs exist for the claims ChiroTouch shows as sent.
- Payer-side enrollment documentation — to verify the practice is still recognized by Medicare, Medicaid, and commercial payers under the current NPI, Tax ID, and PTAN, and that electronic submission is still active at each.
A billing operation that only works inside ChiroTouch can't validate the other two. That isn't a criticism. It's the scope of the work.
The reason ChiroTouch Cloud Specialists exist as a distinct capability is because cross-system migration work is its own discipline — separate from everyday billing, and required in a specific window.
If Your First Question Is "What Does It Cost?" — This Section Is For You
If rate is the first thing a practice asks about migration rescue, it's the wrong first question.
Not because the question is wrong on its own. Because the answer doesn't tell you anything useful about whether your claims are still recoverable. Rate tells you cost. Process tells you outcome. Those are different conversations, and they don't substitute for each other.
Practices that skip the process conversation usually pay for the first audit that didn't work, and then again for the one that does. That's not a rate problem. That's a scope problem — built into how the first audit was purchased.
This is for practices ready to evaluate fit, not just fees. If the whole decision comes down to dollars per claim or percentage of collections without any reference to what's actually getting recovered and how, we're not the right call. And that's fine — we'd rather be clear about it upfront than sort it out in month four.
What the Audit Produces
A completed migration audit hands the practice four specific artifacts:
- A reconciled claim status report — what ChiroTouch says vs. what the clearinghouse says vs. what actually paid.
- A credential-by-credential remediation list — every identifier that needs re-verification, re-registration, or re-authentication, with ownership assigned.
- A recovery timeline ranked by timely filing exposure — which claims need work this week vs. next month vs. aren't coming back at all.
- A prevention checklist for the next migration or software update — the credential map the practice didn't have going into this one.
The value isn't in finding problems. It's in knowing which ones are still recoverable, in what order, by when.
That's also how practices start identifying revenue leakage that existed long before the migration — and only became visible because the migration forced a real reconciliation for the first time.
| Audit Component | In-House Scope | Specialized Audit Scope |
|---|---|---|
| ChiroTouch ledger review | Yes | Yes |
| Clearinghouse reconciliation | Limited | Full — every stalled claim cross-checked |
| Payer enrollment verification | Rarely | Yes — each enrollment validated separately |
| API / OAuth token state audit | No | Yes |
| ERA sub-ID mapping repair | Rarely | Yes |
| MFA / batch automation configuration | No | Yes |
| Timely filing prioritization | Sometimes | Yes — sequenced by risk and recoverability |
Frequently Asked Questions
Why are my ChiroTouch claims "Pending Submission" for weeks after migrating to the Cloud?
Most often, because the OAuth 2.0 handshake between ChiroTouch Cloud and your clearinghouse was never completed, or was completed but never approved on the clearinghouse side. The claim gets packaged and queued inside ChiroTouch but can't authenticate to transmit.
A secondary cause is MFA configuration blocking the automated batch submission script. The software initiates the send, the job hits a security prompt with no user present to respond, and the script times out without logging anything useful. Both of those conditions need admin-level configuration changes at the Cloud layer, not adjustments in the main ChiroTouch UI.
Check the clearinghouse-side submission log first. If there's no record on their side for a claim that shows "Pending Submission" on yours, the break isn't in the claim. It's in the authentication layer.
How do I fix the NPI mismatch error in ChiroTouch Advanced Accounting?
Fixing it requires verification at both ends of the connection — inside the Maintain Trading Partners section of the Accounting application in ChiroTouch, and on your clearinghouse's enrollment record for the practice. The NPI field in ChiroTouch must match the NPI on file at TriZetto, Change Healthcare, or whichever clearinghouse you use, and both must match what Medicare, Medicaid, and your commercial payers have on file for electronic submission.
A mismatch at any point in that chain breaks the whole chain. The practical fix is a side-by-side verification pass. Pull the NPI value from ChiroTouch. Pull it from the clearinghouse portal. Pull it from your most recent Medicare enrollment documentation. Confirm all three are identical. Wherever they aren't, re-register.
None of this takes exotic expertise. It takes access to all three systems at the same time and a willingness to work through the list methodically.
Why are my ERA files not posting automatically after my ChiroTouch Cloud migration?
The migration often resets or corrupts the sub-IDs that map each payer's ERAs to your practice's enrollment inside ChiroTouch. The file arrives at the clearinghouse. The clearinghouse sends it to ChiroTouch. ChiroTouch doesn't recognize the mapping and either drops the ERA entirely or posts it to the wrong claim.
Fixing it means re-verifying ERA enrollment at each payer and rebuilding the sub-ID mapping inside the Cloud configuration. That's not something the clearinghouse can do on their own, and it's not something ChiroTouch support can do without the practice's enrollment records in hand.
Until the mapping gets rebuilt, manual ERA posting is the short-term workaround. It doesn't scale, and it creates its own reconciliation problems if it runs for more than a few weeks. The real fix is the mapping.
Do I need new TriZetto login credentials for ChiroTouch Cloud in 2026?
Logins aren't the issue. Re-authentication is. Your TriZetto username and password almost certainly still work at the portal level. The break happens at the API layer, where ChiroTouch Cloud talks to TriZetto through OAuth 2.0 tokens that have to be regenerated and approved separately from user login credentials.
Think of it as two connections. The person logging in is one. The software talking to other software is the other. A migration can complete the first connection without completing the second — which is why a practice can log in, see everything looking normal, and still have zero claims actually transmitting.
Resolving it takes coordination between your ChiroTouch Cloud admin and TriZetto support to regenerate the tokens and confirm they've been authorized on both sides. Not complicated work. Just not something anyone does automatically.
How do I re-verify my Medicare Provider ID in the new ChiroTouch interface?
Verification happens in three places, not one. Inside ChiroTouch, check each provider's Medicare identifiers in the Accounting module against the practice's current PTAN and NPI records. At the clearinghouse, confirm Medicare enrollment is still active and that the EDI submission channel is configured correctly.
At CMS, confirm the practice's PECOS enrollment is current and that the MBI format your Cloud instance transmits matches the current CMS standard. Any one of those three being stale produces Medicare rejections that don't always route back in a way you can actually see.
Rejections that don't post as rejections — because the ERA mapping is also broken — are the worst version of this problem. The claim stays unresolved indefinitely while nothing actionable appears inside the software.
Can I just revert back to ChiroTouch Server if the Cloud migration breaks my billing?
In most cases, no. Once the Cloud migration completes, the Server version of the clinic's data is typically frozen and no longer supported as a live operating environment. Reverting introduces data continuity risks that are usually worse than the migration issues themselves.
The more useful question is whether the migration can be finished properly — because in most cases, the Cloud environment is technically functional. What's broken is the credentialing layer between ChiroTouch and the clearinghouse, and that can be rebuilt without undoing the move.
Reversion is almost never the answer. Proper credential reconciliation almost always is. The instinct to go backward is understandable, but it usually costs more than it saves.
Should I just wait for ChiroTouch to push a software fix through their support portal?
Waiting treats this as a software problem. It isn't. The majority of Cloud migration billing interruptions happen at the credential and protocol layer — outside what ChiroTouch's software patches can reach.
ChiroTouch can fix bugs inside their application. They can't re-register your NPI with your clearinghouse. They can't re-authenticate your API tokens. They can't re-enroll your ERAs with each payer. Those tasks live at the clearinghouse and payer level, and they require direct action from the practice or its billing partner.
Waiting for a software fix to solve credential work is how claims age past timely filing. The fix is coordinated credential reconciliation, and it starts the day the migration goes live — not the day AR crosses a threshold that finally gets somebody's attention.
The Migration Is a Credentialing Project, Not a Software Update
The practices that recover fastest from a ChiroTouch Cloud migration all do one thing in common. They stop treating it as a software event.
Every identifier connecting the practice to the people paying its claims has to be re-verified, re-authenticated, or rebuilt on the new protocol. Waiting doesn't make that work simpler. It makes it harder, because claims keep aging while the credentials stay broken.
The practices that came through clean in early 2026 did three things differently from everyone else:
- Audited every credential before the server came down — not after. The credential map existed before migration day, not as a post-mortem.
- Reconciled the Cloud ledger against clearinghouse logs in the first two weeks — not the first two months. Discrepancies got caught while claims were still inside timely filing windows.
- Treated the migration as a project that owed them specific artifacts — a reconciled status report, a remediation list, a recovery timeline. Not a software update that would settle on its own.
The clinics still running silent six weeks later almost all made the same assumption. That the software would sort it out.
The software is the software. The credentials are a different job. Both of them have to be handled, and only one of them is actually ChiroTouch's problem to solve.
Whichever stage your practice is in right now, the recovery starts in the same place — with a reconciliation that tells you what's still workable, what isn't, and what it takes to make the Cloud instance a reliable transmission channel from here forward.
A ChiroTouch Cloud migration resets more than software. It resets every credential, every Trading Partner ID, and every authentication protocol sitting between your practice and the people paying your claims.
A practice assessment shows you what's actually transmitting, what's stuck in "Pending Submission," and which credentials need to be rebuilt before more claims age past the point of recovery.
Book a review of your post-migration billing state.
Practices that came through this migration cleanly didn't wait for the software to settle, and they didn't wait for support to find the gap on their behalf. They reconciled the environment themselves, and kept their software specialists accountable for the handoff.
© 2026 Bushido Billing. All Rights Reserved | Web Design by iTech Valet


