How to Transition from "Survival Billing" to Wealth-Building Cycles in 2026
The difference between survival billing and wealth-building cycles comes down to one thing: systems. Survival billing means reacting to problems as they appear. Wealth-building means having processes in place that prevent most problems from happening in the first place.
If your billing feels unpredictable right now, you're in good company. Many practice owners find themselves in a reactive pattern—checking the bank account before payroll, wondering when claims will pay, spending evenings catching up on denials. This isn't a personal failure. It's usually the natural result of a growing practice without matching growth in billing infrastructure.
Here's what we know from working with practices across the country: research indicates that 30% of chiropractic claims are denied on first submission, and each reworked claim adds roughly $50 in staff time and administrative costs. That adds up quickly, but the good news is that most of those denials are preventable with the right systems.
The shift from reactive to proactive billing isn't complicated, but it does require intentional changes. It means implementing standardized processes, tracking specific metrics, and treating your revenue cycle as something worth protecting rather than just an administrative task to get through.
In 2026, with Medicare conversion factor increases of 3.26% and evolving payer requirements, practices with systematic billing will be positioned to capture those opportunities. The practices reducing chiropractic denial rates through proactive approaches typically recover 60-70% of previously missed revenue within the first few months.
This article walks through what that transition looks like, step by step.
Understanding How Practices End Up in Survival Mode
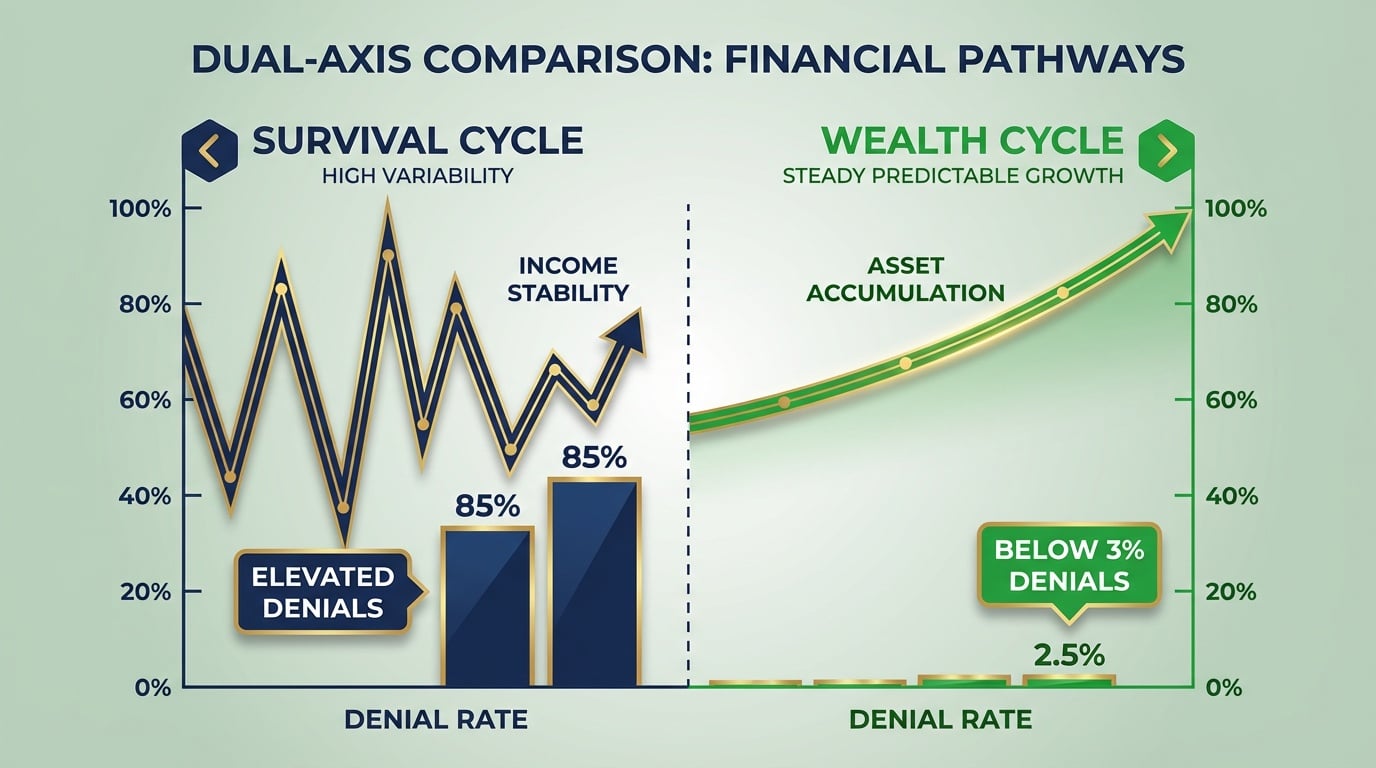
Most practice owners don't set out to run reactive billing operations. It happens gradually, usually through a combination of growth, staff changes, and the daily demands of patient care.
The pattern typically looks something like this: billing starts out manageable, then patient volume increases, then the person handling billing gets stretched thin, then claims start taking longer to follow up on, and before long the focus shifts from preventing denials to cleaning up after them.
Understanding how this happens helps you see where the leverage points are for making changes.
The Real Cost of Reactive Billing
When billing becomes reactive, practices tend to lose revenue in ways that aren't always visible on a monthly report. These losses accumulate through several channels.
- Denials that don't get appealed - When the workload is high, some denied claims simply don't get the attention they need. A 2025 billing compliance study found that practices with systematic denial management recover claims that otherwise would have been written off.
- Aging accounts - The MGMA benchmark for AR over 90 days is around 13.5%. When billing is reactive, that percentage tends to climb, and older claims become harder to collect.
- Staff capacity - When your team spends time identifying revenue leakage and chasing old claims, that's time not spent on prevention or other high-value work.
Opportunity costs - Hours spent reworking claims are hours that could go toward denial prevention, patient care coordination, or growth initiatives.
Why Adding More Effort Doesn't Always Help
The natural response when billing falls behind is to work harder—longer hours, weekend catch-up sessions, maybe hiring additional help. But when the underlying processes are the issue, more effort within those same processes only provides temporary relief.
Here's what we see often: someone stays late to resubmit denied claims and successfully collects on some of them. But while they're focused on yesterday's denials, today's claims go out without the verification steps that would prevent tomorrow's denials. The pattern continues.
The path forward isn't necessarily more effort. It's different effort—effort applied to building systems that prevent problems rather than effort applied to resolving them after they occur.
Assessing Where You Are Now
Most practice owners have a general sense of how their billing is going, but it helps to look at specific indicators. Here's a framework for assessing your current position.
| INDICATOR | REACTIVE RANGE | TRANSITIONAL RANGE | SYSTEMATIC RANGE |
|---|---|---|---|
| Days in AR | 45+ days | 31-44 days | Under 30 days |
| Net Collection Ratio | Below 94% | 94-95% | 96%+ |
| Denial Rate | Above 12% | 9-12% | Below 8% |
| AR Over 90 Days | Above 18% | 14-17% | Below 13.5% |
| Cash Flow Predictability | Highly variable | Highly variable | Consistent month-to-month |
If several of these place you in the reactive range, there's likely room for meaningful improvement. And that's genuinely good news—it means there's recoverable revenue available.
The Wealth-Building Transition Checklist
| COMPONENT | SURVIVAL BILLING (REACTIVE) | WEALTH-BUILDING (SYSTEMATIC) |
|---|---|---|
| Verification | After denial or at point of sale | 48 hours before appointment |
| Documentation | Weekends or late nights | Same-day with real-time review |
| Submission | When the pile gets high | Within 72 hours of service |
| Follow-up | When cash is low | Defined 14/21/35 day intervals |
| Visibility | Monthly bank statement | Weekly KPI dashboard |
The Wealth-Building Approach

Wealth-building billing focuses on prevention rather than recovery. Instead of asking "how do we get paid on this claim," the question becomes "how do we make sure this claim pays correctly the first time."
This shift changes how you approach every part of your revenue cycle, from scheduling through final payment posting.
Moving from Reactive to Proactive
Proactive billing means addressing potential issues before claims are submitted. This involves attention at each stage of the process.
- Pre-appointment verification - Confirming insurance eligibility and benefits before the patient arrives, not after services are rendered. Real-time eligibility verification helps prevent coverage surprises that create collection challenges.
- Same-day documentation - Making sure clinical notes support billing codes before the claim is generated. Improper modifier usage accounts for 31% of chiropractic claim denials, and most of these stem from documentation gaps.
- Pre-submission review - Running claims through automated checks that catch coding errors, missing information, and payer-specific requirements before submission.
- Consistent follow-up - Following unpaid claims at defined intervals rather than when time allows.
Building a KPI Dashboard
Practices that build wealth through billing track specific metrics regularly. The difference isn't just measurement—it's using those measurements to make decisions before small issues grow.
Your core KPI dashboard should include these metrics, reviewed weekly.
| METRIC | CALCULATION | TARGET | WHEN TO INVESTIGATE |
|---|---|---|---|
| Clean Claim Rate | Claims passing all edits / Total claims submitted | Above 95% | Below 93% |
| First-Pass Resolution | Claims paid on first submission / Total claims | Above 90% | Below 85% |
| Days in AR | Total AR / Average daily charges | Under 30 | Above 40 |
| Net Collection Ratio | Collections / Collectible charges | 96%+ | Below 95% |
| Denial Rate | Denied claims / Total claims | Under 8% | Above 10% |
The Revenue Protection Mindset
Practices with strong billing treat the function as a strategic asset that requires specialized attention. This might mean developing internal expertise, partnering with billing specialists, or combining both approaches.
The key distinction is between passive claim submission and active revenue protection. Passive submission means sending claims out and waiting to see what happens. Active revenue protection means every claim goes out correctly, every denial gets prompt attention, and every dollar earned gets collected.
This approach requires someone—whether internal or external—who understands chiropractic-specific billing requirements, knows payer nuances, and has the capacity for consistent follow-through. The human judgment in billing that experienced specialists bring complements what software can do, particularly for complex cases involving Medicare compliance and personal injury claims.
The 2026 Billing Environment
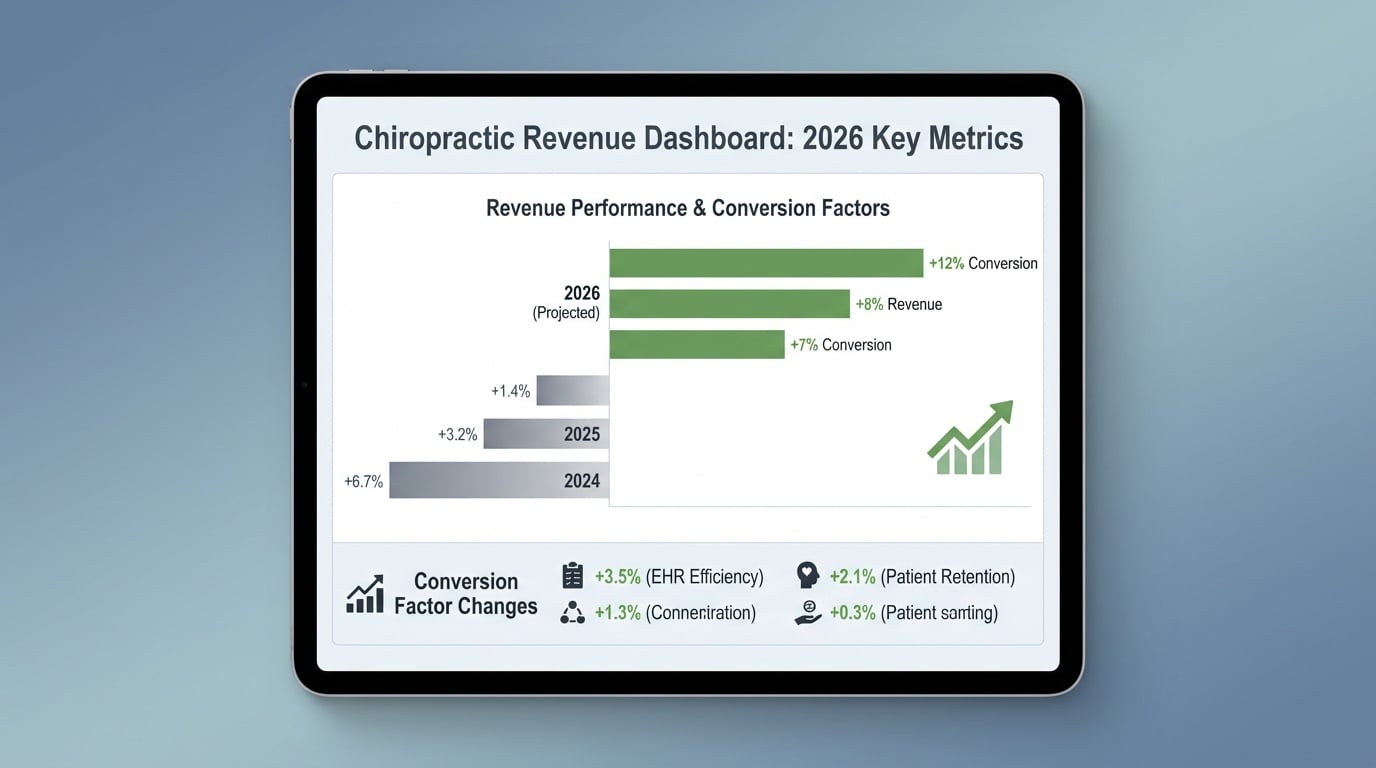
Understanding the current regulatory and payer environment helps you position your practice for the year ahead. 2026 brings some positive changes along with increased complexity.
Medicare Payment Updates
The CY 2026 Medicare Physician Fee Schedule introduces several changes relevant to chiropractic reimbursement.
For the first time, CMS is implementing two separate conversion factors. Qualifying APM participants receive $33.57 (a 3.77% increase), while other practitioners receive $33.40 (a 3.26% increase). This is an improvement from the $32.35 conversion factor in 2025, though capturing the full benefit requires clean claims and proper documentation.
The rule also finalizes an efficiency adjustment of -2.5% to work RVUs for non-time-based services. For chiropractic practices, this means documentation supporting medical necessity remains essential. Medicare's "Documentation Compliance Audit Initiative" continues to focus on chiropractic providers, with post-payment reviews examining the distinction between active treatment and maintenance care.
- AT modifier requirements - Still required for all Medicare spinal manipulation claims (98940-98942). Claims without it are automatically classified as "maintenance therapy."
- Documentation standards - Should include initial treatment plan with measurable goals, functional improvement documentation, and re-evaluation notes at regular intervals.
- Subluxation documentation - Requires specific objective findings including motion palpation results and baseline comparisons.
Payer Automation
Insurance companies increasingly use automated systems to review claims before human review. According to HFMA research on claim integrity, this has changed denial patterns across the healthcare industry.
The Kaufman Hall 2025 Health System Performance Outlook found that 44% of healthcare organizations cite denial rates and administrative burden as their top managed care concerns. Front-end issues—authorization, eligibility, and benefits verification—lead the list of denial contributors at 26%.
For chiropractic practices, this means:
- Automated claim review - Payer systems flag documentation gaps, modifier issues, and frequency patterns quickly. Claims that might have passed review a few years ago now get flagged by automated systems.
- Medical necessity review - Automated systems cross-reference treatment frequency against diagnosis codes and flag patterns suggesting maintenance rather than active care.
- Modifier verification - Automated checks confirm AT modifier presence and alignment with supporting documentation.
Patient Responsibility
The growth of high-deductible health plans has shifted more of the collection responsibility to providers. According to KFF research, 87% of covered workers had a general annual deductible in 2024, with an average single deductible of $1,787. Over 32% of workers have deductibles exceeding $2,000.
This creates a balancing act: collecting from patients who owe more while maintaining the relationships that keep them coming back. Securing predictable clinic cash flow requires attention to both the financial and relational aspects.
Practices handling this well tend to focus on:
- Upfront cost communication - Calculating patient responsibility before services and discussing it clearly.
- Time-of-service collection - Collecting patient portions while patients are still in the office.
- Payment options - Offering payment plans that increase collection rates while respecting patient circumstances.
- Plain language - Explaining insurance coverage and patient responsibility in straightforward terms.
Implementing Systematic Processes
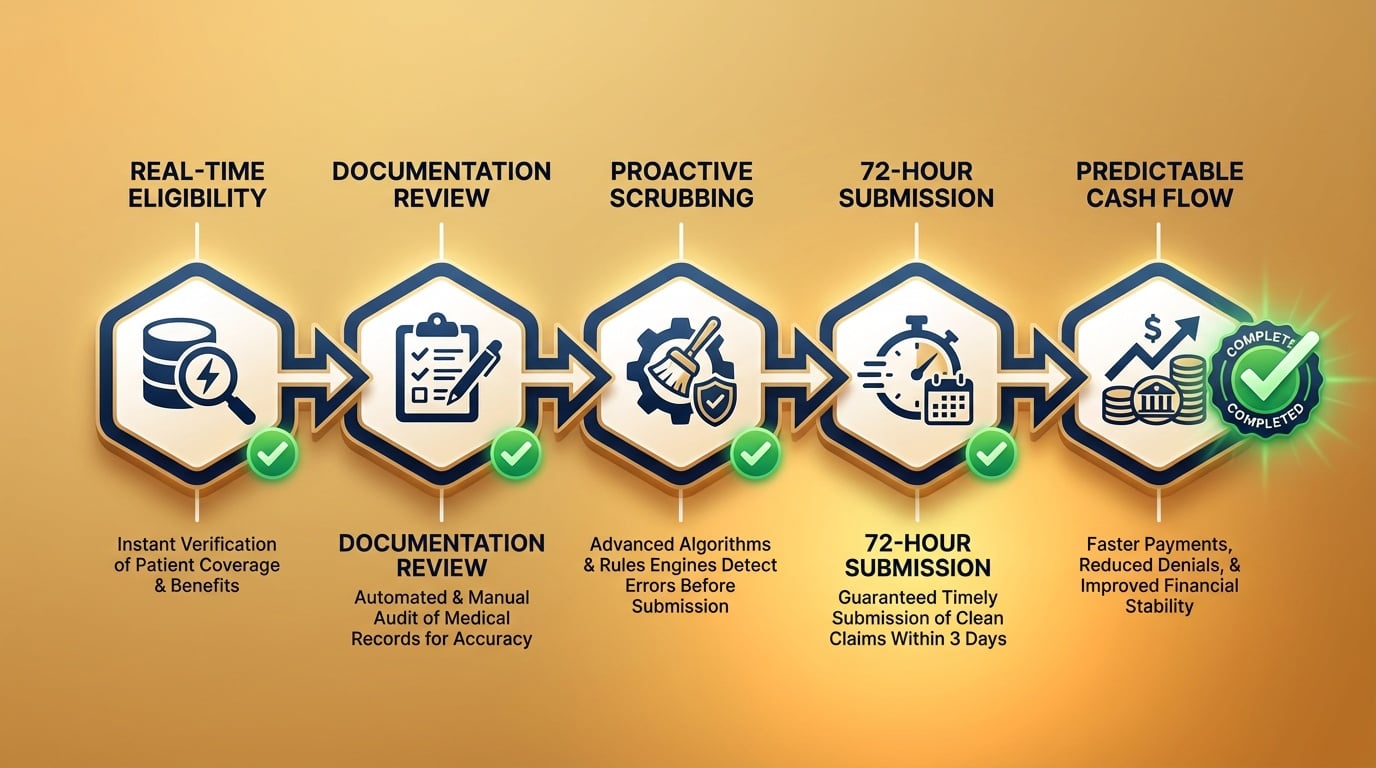
Building Clean Claim Capability
Clean claims—those submitted without errors requiring rework—form the foundation of efficient billing. The MGMA benchmark for first-pass resolution suggests that practices should aim for at least 90% of claims paid on first submission.
Building this capability requires standardizing each step before submission.
- Eligibility verification protocol - Verify insurance 48 hours before scheduled appointments. Confirm coverage specifics including chiropractic benefits, visit limits, and authorization requirements. Document verification in the patient record.
- Documentation review checklist - Before generating claims, confirm diagnosis codes match documented conditions, treatment codes align with services performed, modifiers are appropriate and supported by documentation, and all required fields are complete.
- Claim review workflow - Run all claims through automated review before submission. Address flagged items before submission. Track patterns in flagged items to identify training opportunities.
- Submission timing - Submit clean claims within 72 hours of service date. Delayed submission extends the collection timeline and can increase denial risk.
Denial Prevention
Preventing denials takes less effort than managing them. A systematic prevention approach addresses the most common denial categories before they occur.
AR Management
| DENIAL CATEGORY | PREVENTION ACTION | FREQUENCY |
|---|---|---|
| Frequency | Real-time verification | Every appointment |
| Authorization | Pre-service confirmation | Procedures/new patients |
| Medical Necessity | Documentation review | Every claim |
| Coding Errors | Automated review | Every submission |
| Timely Filing | Submission monitoring | Daily |
| Duplicate Claims | System checks | Every submission |
For chiropractic practices specifically, the AT modifier and medical necessity documentation deserve particular attention. Research from the American Chiropractic Association indicates that practices implementing structured documentation protocols see denial reductions of 25-40%.
Even with strong prevention, some claims need follow-up. Systematic AR management ensures claims get attention at appropriate intervals.
A typical workflow operates on defined intervals:
- Day 14 - Confirm claim receipt by payer. Resubmit missing claims promptly.
- Day 21 - First follow-up on unpaid claims. Identify and address any issues flagged by payer.
- Day 35 - Second follow-up with escalation for unresolved issues. Begin appeal process if denial received.
- Day 45 - Supervisor review of all claims reaching this threshold. Look for patterns in what's aging.
- Day 60 - Final collection efforts before moving to additional measures.
The discipline of consistent follow-up at defined intervals makes a significant difference in collection outcomes.
Measuring Progress
Transitioning toward wealth-building billing takes time. Tracking the right metrics helps you confirm progress, identify areas needing attention, and maintain momentum through the change.
Monthly Review Focus
Your monthly billing review should focus on trends rather than isolated data points. Consistent improvement matters more than hitting perfect numbers immediately.
- Collection speed - Track how quickly payments arrive after claim submission. Improvement here indicates cleaner claims and better follow-up.
- Denial rate by category - Separate denials into preventable (coding, eligibility, authorization) and less preventable (policy exclusions, maximum benefits). Focus improvement efforts on preventable categories.
- Days in AR trend - Watch the overall trend and the distribution. Reducing claims in the 60-90 day range matters as much as the headline number.
- Cost to collect - According to HFMA's definition, this is total revenue cycle cost divided by patient service cash collected. As efficiency improves, this ratio should decline.
Staff workload - Track claims processed per hour and follow-up activities completed. Improving systems should increase throughput while reducing stress.
Benchmark Reference
Comparing your metrics against industry standards helps you understand where you stand relative to peers. This table provides reference points for chiropractic and allied health practices in 2026.
| METRIC | BELOW BENCHMARK | AT BENCHMARK | ABOVE BENCHMARK |
|---|---|---|---|
| Days in AR | 50+ days | 35-49 days | Under 35 days |
| Net Collection Ratio | Below 93% | 93-95% | Above 96% |
| Denial Rate | Above 12% | 8-12% | Below 8% |
| Clean Claim Rate | Below 90% | 90-94% | Above 95% |
| AR Over 90 Days | Above 20% | 14-19% | Below 13.5% |
| First-Pass Resolution | Below 85% | 85-89% | Above 90% |
Improving just two or three metrics from below benchmark to at or above benchmark typically represents meaningful revenue recovery.
Realistic Timeline
Knowing what to expect helps you stay committed through the transition. Most practices see improvement in a general pattern:
- Months 1-2 - Process implementation, training, and baseline establishment. Metrics may shift during the adjustment period.
- Months 3-4 - Clean claim rate improvements become visible. Denial rate begins declining as prevention protocols take effect.
- Months 5-6 - Days in AR starts declining as cleaner claims move through the system faster. Cash flow becomes more predictable.
- Months 7-12 - Compounding effects create sustained improvement. Staff workload shifts from reactive to proactive. Margins improve.
The transition requires patience and consistent execution. Practices that stick with systematic changes see meaningful results.
Building Your Support Structure

Most practices benefit from some form of support in making this transition. The question is what kind of support structure fits your situation, resources, and goals.
Developing Internal Capability
If building internal capabilities, focus development on these core areas:
- Coding expertise - Someone who deeply understands chiropractic-specific CPT and ICD-10 coding, including AT modifier requirements and medical necessity documentation standards.
- Payer knowledge - Each major payer has specific requirements and preferences. This knowledge takes time to accumulate and requires ongoing updating.
- Follow-up consistency - AR management requires someone willing to make calls, navigate payer systems, and work toward resolution day after day.
- Analytics capability - Tracking and interpreting KPIs requires comfort with data and the ability to translate numbers into actionable insights.
Building all these capabilities internally requires investment in training, sufficient staff depth for coverage, and ongoing development to maintain current knowledge.
Evaluating Partners
Specialized billing partners can support the transition by bringing expertise and systems that have been refined over time. Evaluating potential partners involves looking at specific capabilities.
- Specialty focus - Partners specializing in chiropractic and allied health understand the billing challenges specific to your practice. Generalist services may miss chiropractic-specific requirements.
- Platform flexibility - The best partners work with your existing EHR—Jane App, ChiroTouch, Genesis, or others—rather than requiring software changes.
- Transparency - You should have visibility into claim status, denial reasons, and collection activities. Clear reporting and accessible communication matter.
- Communication standards - Regular reporting and responsive contacts help when questions arise or issues need attention.
Pricing alignment - Performance-based pricing aligns interests—your partner does well when you do well.
Combining Approaches
Many practices find success combining internal resources with external expertise. The front desk handles patient registration and eligibility verification while billing specialists manage claim submission, follow-up, and denial resolution.
This approach keeps patient-facing functions internal while drawing on specialized expertise for technical billing work. It also provides coverage that pure internal teams may lack—if your office manager is out, billing continues without interruption.
The right structure depends on your practice size, growth plans, patient volume, and the expertise available in your area.
Frequently Asked Questions
What is the difference between a gross collection ratio and a net collection ratio?
Gross collection ratio measures total payments received divided by total charges billed. Net collection ratio measures payments received divided by the amount you were actually entitled to collect after contractual adjustments.
A practice might have a 60% gross collection ratio but a 96% net collection ratio. The difference comes from contractual adjustments—the amounts you agreed to accept from insurance companies. If you bill $100 but your contracted rate is $60, and you collect $58, your gross ratio is 58% but your net ratio is about 97%.
Net collection ratio is the more meaningful metric because it shows how effectively you capture every dollar you've earned under your contracts.
How do I know if my chiropractic practice is in 'Survival Billing' mode?
Signs of survival billing extend beyond financial metrics to how billing feels day-to-day. You may be in survival mode if you find yourself checking your bank account before major purchases to confirm funds are available.
Other indicators include unpredictable cash flow from month to month, spending evenings or weekends catching up on billing, AR over 90 days exceeding 15% of total receivables, denial rates above 10%, and feeling uncertain about when and whether claims will pay.
The operational feel matters too. If billing creates more stress than confidence, if it feels reactive rather than organized, that's usually a signal there's room for systematic improvement.
What are the 2026 benchmarks for a healthy chiropractic practice?
Key 2026 benchmarks provide reference points for assessing billing performance. For practices with high volumes of office visits, MGMA guidelines suggest Days in AR should be under 30 days.
Additional benchmarks include net collection ratio of 96% or higher, denial rate below 8-10%, clean claim rate above 95%, first-pass resolution rate above 90%, and AR over 90 days below 13.5% of total receivables.
Meeting these benchmarks indicates your practice has moved toward systematic, wealth-building operations. The numbers reflect underlying processes that create predictable cash flow and protected margins.
Does outsourcing billing help build practice wealth?
Outsourcing can support wealth building when partnered with a billing company that understands chiropractic-specific requirements. The right partner brings systematic processes, denial prevention expertise, and consistent follow-up capacity.
The key is choosing a partner who focuses on your specific specialty rather than taking a generalist approach. Chiropractic billing has unique requirements—AT modifier rules, medical necessity documentation, maintenance care distinctions—that require specialized knowledge.
Outsourcing tends to make particular sense when internal team changes disrupt billing continuity, when growth has outpaced current billing capacity, or when you'd prefer to direct administrative time toward patient care and practice development.
How can I reduce my Days in AR to under 30 days?
Reducing Days in AR involves improvement at each stage of the revenue cycle, not just faster follow-up. Start by submitting clean claims within 72 hours of service date. Delayed submission extends the collection timeline before it begins.
Verify insurance eligibility before appointments to prevent coverage issues that delay payment. Use correct modifiers consistently and ensure documentation supports every code billed. Follow up on unpaid claims at regular intervals rather than waiting for aging reports.
Address denials promptly when they arrive. Quick response prevents denials from aging into harder-to-collect receivables. Track denial patterns and implement prevention measures for issues that recur.
Why is my office manager's burnout linked to our AR aging report?
When AR ages beyond 60-90 days, collection becomes more labor-intensive. Claims beyond 60 days have lower recovery rates and require more follow-up calls, documentation gathering, and appeals.
This creates a situation where your office manager spends increasing time on difficult collections instead of maintaining current workflows. The workload compounds because time spent on older claims means less time for prevention, which can lead to more claims aging.
Addressing this pattern usually requires systematic changes that reduce inflow into older aging buckets, not just faster work on the existing pile.
How do I calculate the 'Cost to Collect' in my clinic?
Cost to collect is calculated by dividing your total revenue cycle costs by total cash collected during the same period. Revenue cycle costs include staff wages dedicated to billing functions, billing software and clearinghouse fees, outsourced billing services, supplies, and overhead allocations.
The HFMA definition includes all operational costs required to process and collect payment. You can calculate it with or without IT infrastructure costs depending on your preference.
Tracking this metric helps you understand the efficiency of your billing operations. As systems improve, cost to collect should decline even as total collections improve.
Can I build wealth while still taking insurance in 2026?
Yes. Insurance-based practices can achieve strong margins through disciplined revenue cycle management. Practices that implement systematic processes, track the right KPIs, and maintain clean claim rates above 95% do well financially while accepting insurance.
The key is treating billing as a strategic function rather than just something to get through. The challenges of insurance billing are real, but they're manageable with the right approach.
Cash-pay practices have simpler billing but often trade off patient volume and predictable flow. The wealth-building opportunity for insurance-based practices lies in maximizing collection efficiency while maintaining patient relationships.
Taking the Next Step
The shift from survival billing to wealth-building is one of the more meaningful changes a practice owner can make. It affects cash flow, day-to-day stress, growth capacity, and the long-term stability of the practice.
The path involves implementing systematic processes that prevent problems, tracking metrics that provide early signals, and building support structures—internal, external, or combined—that provide the expertise and consistency your billing requires.
2026 brings opportunities for practices that approach billing systematically. The Medicare updates, payer automation trends, and patient responsibility shifts all favor organized operations.
The steps are straightforward even if they require consistent attention: start with where you are, implement what you can, and build from there. Small improvements compound over time into meaningful results.
If you're thinking "this makes sense, but I'm not sure where to start," we understand. Most clinic owners we talk with feel the same way at first.
That's why we offer a free discovery call. It's a conversation about your current billing situation—what's working, what could be better, and what options might fit.
We'll help you understand:
- Where claims might be getting stuck in your current process
- What's behind any denials or delays you're seeing
- Whether your AR is in good shape or needs some attention
- How your current approach compares to what we typically see
- What working with a billing partner would actually involve
Book a Call — no pressure, just a straightforward conversation about your billing.
We're happy to talk through your situation and help you figure out next steps, whether that involves working with us or not.
© 2026 Bushido Billing. All Rights Reserved | Web Design by iTech Valet


