Flat Fee vs. Percentage-Based Billing: Which Model Protects Your 2026 Revenue?
Optimizing ChiroTouch for faster claim processing in 2026 comes down to three things: activating the automation that's already built into the platform, making sure your clearinghouse integration is configured correctly, and using Rheo AI's compliance tools to catch documentation issues before they turn into denials.
ChiroTouch has a lot of capability built in. Between Rheo AI, integrated clearinghouses, automated scrubbing, and real-time eligibility verification, the tools for fast, clean billing are already there. The challenge is that most practices set up their workflow during onboarding and haven't revisited it since, even as the software and payer requirements have changed around them.
That's understandable. You're running a clinic, seeing patients, and managing a team. Billing configuration usually isn't the thing that gets your attention until something goes wrong.
This guide walks through the specific settings, integrations, and workflows that help ChiroTouch practices move from delayed claim cycles to consistent, same-day submissions. Whether you're on ChiroTouch Cloud or still running the server-based version, there are practical steps you can take to get claims out the door faster and keep your revenue cycle moving.
And if your billing workflow feels more reactive than proactive — more focused on identifying revenue leakage after the fact than preventing it — that's a clear sign the configuration deserves a closer look.
The goal here is straightforward: securing predictable clinic cash flow so billing stops being a source of stress and starts working quietly in the background, the way it should.
Why Your ChiroTouch Workflow Might Need a Tune-Up
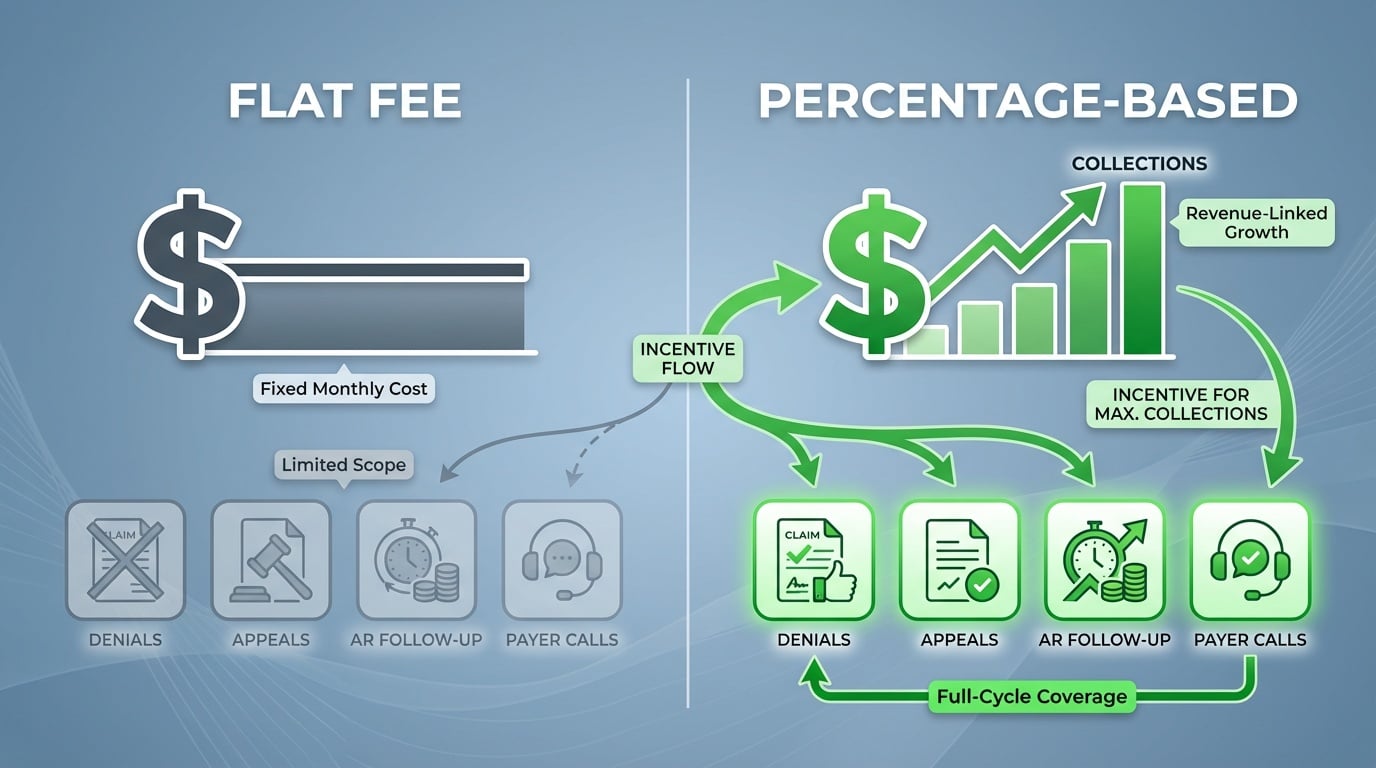
Flat Fee: The Fixed Monthly Rate
A flat-fee billing model charges your practice a set dollar amount each month—typically ranging from $1,000 to $3,000 or more, depending on claim volume and services included.
The appeal is straightforward. You know exactly what billing costs every month, regardless of collections. For a clinic owner managing a tight budget, that consistency can feel reassuring.
The trade-off is that your billing company's revenue stays the same whether your collections are $40,000 or $80,000 in a given month. Their income isn't affected by how many claims are collected or how quickly AR is resolved.
This means there's no built-in financial reason for the billing company to:
- Spend extra time on complex denials and appeals
- Pursue low-dollar claims that require significant follow-up
- Invest in payer-specific research for tricky modifiers
- Proactively call payers to resolve held claims
That doesn't mean flat-fee billing companies don't do these things. Many do. But the structure itself doesn't reward that effort, and over time, that can affect how consistently the harder work gets done.
The Hybrid Model
Some billing companies use a hybrid structure: a smaller base fee combined with a reduced percentage of collections. This can work well for practices with seasonal volume changes or during a transitional period.
The key question with any hybrid is still the same: does the structure create shared accountability? If the base fee is high enough that the billing company can operate comfortably regardless of collections, the hybrid functions more like a flat fee with a different label.
| Feature | Flat Fee | Percentage-Based | Hybrid |
|---|---|---|---|
| Monthly Cost | Fixed ($1,000–$3,000+) | Variable (5–10% of collections) | Base fee + reduced percentage |
| Incentive Alignment | Limited—paid regardless of outcome | Strong—revenue tied to performance | Depends on the base-to-percentage balance |
| Denial Follow-Up | Often limited or excluded | Part of the standard process | Varies by contract |
| Best For | Low-volume practices with simple claims | Practices focused on growth and collections | Practices with seasonal volume changes |
Understanding the Full Cost of Your Billing Model

Unworked Claims
This one is less visible but equally important.
In any billing operation, some claims require more effort than others. A clean $200 evaluation code processes quickly. A denied $45 spinal manipulation claim with a modifier issue might take 30 minutes of phone time with the payer.
Under a flat-fee model, both claims generate the same revenue for the billing company—none, directly. So there's no financial distinction between resolving the easy claim and resolving the hard one.
Under a percentage model, every collected dollar counts. Over a full month, hundreds of smaller claims represent meaningful revenue for the billing partner. That financial reality tends to keep those claims from being deprioritized.
This isn't about any billing company intentionally neglecting claims. It's about what the structure naturally encourages over time.
The Full Cost-to-Collect Picture
The healthcare industry tracks billing efficiency through a metric called "cost to collect." Industry benchmarks place this between 3% and 8% of net patient revenue, depending on practice size, specialty, and billing approach.
Here's how a side-by-side comparison can look when you include the less obvious costs:
| Scenario | Flat Fee | Percentage-Based (7%) |
|---|---|---|
| Monthly Collections | $55,000 | $62,000 |
| Billing Fee | $2,000 | $4,340 |
| Administrative Rework (staff time) | $3,200 | $0 (included in service) |
| True Cost to Collect | $5,200 (9.5%) | $4,340 (7%) |
| Net Revenue After Billing | $49,800 | $57,660 |
The flat fee looks less expensive at the surface level. But when you account for the additional staff time and the collection difference driven by incentive alignment, the net revenue gap is significant.
The difference of $7,860 per month in this scenario reflects what can happen when a billing partner has a consistent financial reason to follow through on every claim.
Why This Decision Matters More in 2026
Denial Rates Continue to Rise
Denial rates have been trending upward for several years now, and the pattern has continued into 2025.
The 2025 State of Claims report from Experian Health found that 41% of healthcare providers now report denial rates above 10%. That's up from 30% in 2022. Additionally, 54% of providers say claim errors are increasing, and 68% say submitting clean claims has become more challenging.
For chiropractic practices, common denial triggers include:
- Medical necessity documentation for maintenance care—especially distinguishing active treatment from maintenance
- Incorrect modifier usage, particularly the AT modifier on Medicare claims
- Gaps in prior authorization or missing referral documentation
- Patient eligibility errors that weren't caught at check-in
A billing partner who shares in the financial outcome of each claim has a clear reason to stay ahead of these patterns—through better claim scrubbing, more thorough documentation review, and consistent payer follow-up.
Medicare Adjustments Add Complexity
The 2026 Medicare conversion factor of $33.40 includes a temporary 2.5% increase from the One Big Beautiful Bill Act. That's a welcome improvement.
But it arrives alongside the CMS efficiency adjustment of -2.5% applied to work RVUs for many procedural codes. For some practices, these changes largely offset each other.
When reimbursement per claim is relatively flat, each unresolved denial or delayed payment has a slightly larger impact on cash flow. A billing partner with a financial stake in collections is more likely to work through these claims systematically—because their own revenue depends on it.
This is where the concept of active revenue defense becomes practical. It's not about urgency. It's about having a billing partner who consistently follows through because the structure supports that behavior.
Payer Processes Are Getting More Automated
Insurance companies are using more automated systems to review and process claims. This has made some aspects of billing faster, but it's also introduced new denial patterns—particularly around medical necessity reviews and documentation requirements.
Automated denial patterns tend to be consistent and recognizable. A billing team that's paying close attention can often identify the pattern and adjust submissions before claims are flagged.
But that level of attention takes time and effort. Under a percentage model, that effort pays off directly because resolved claims generate income for the billing partner. Under a flat fee, the same effort has no impact on the billing company's revenue—which can affect how consistently that proactive work happens.
The key point isn't that flat-fee billers can't do this work. It's that the percentage model creates a sustainable reason for the billing team to invest in it over the long term, which supports securing predictable clinic cash flow.
How to Evaluate Your Current Billing Arrangement
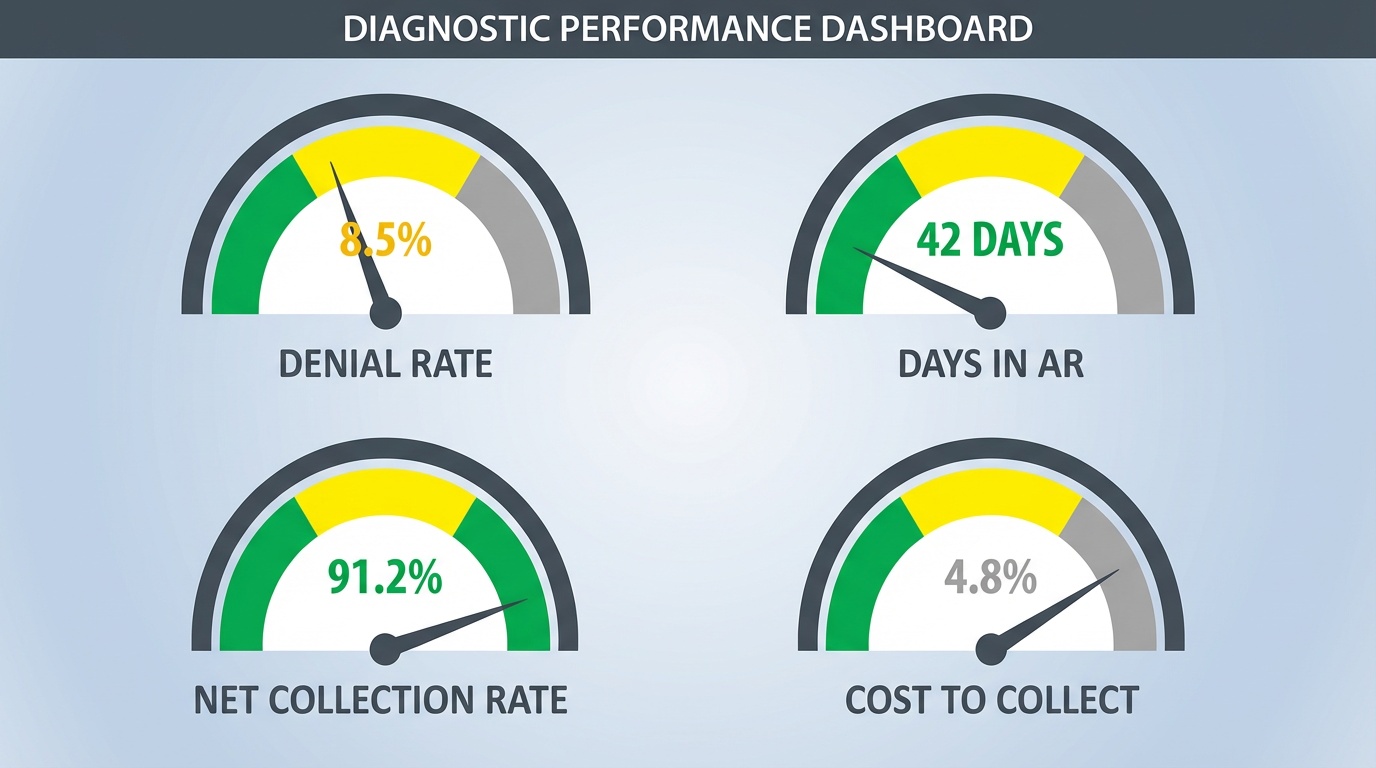
Five Questions Worth Asking Your Billing Company
- What is my current denial rate, and what's the trend over the past 6 months? A reliable billing partner should have this number readily available. Under a percentage model, they're tracking it closely because it affects their own income.
- How much of my AR is over 90 days? Reading an AR aging report regularly is one of the best ways to gauge billing health. Your billing partner should be the one walking you through it—not the other way around.
- What happens after a claim is denied on first submission? Look for specifics. A clear process might include automatic resubmission, payer follow-up calls, and a defined escalation path for complex denials.
- What's included in my fee versus what's billed separately? Some flat-fee contracts charge separately for credentialing, complex appeals, patient billing, and AR cleanup. Understanding the full scope prevents surprises.
- How often do we communicate, and who initiates it? Transparent, consistent communication is a cornerstone of a reliable billing relationship. Weekly reporting and proactive updates should be standard—not something you have to request.
A Simple Self-Assessment
These benchmarks can give you a quick read on where your billing stands today:
| Metric | Healthy Range | Worth Reviewing |
|---|---|---|
| Net Collection Rate | 95–99% | Below 90% |
| Days in AR | Under 35 days | Over 50 days |
| Denial Rate | Below 5% | Above 10% |
| AR Over 120 Days | Less than 10% of total AR | More than 15% |
| Cost to Collect | 3–7% of net revenue | Above 8% |
If a couple of these metrics look off, it doesn't necessarily mean your billing company is doing a poor job. It could be a documentation issue, a payer mix problem, or a coding gap.
But it's worth exploring whether the structure of your billing arrangement is supporting the kind of follow-through these metrics require. Sometimes a model change can improve results without changing the people involved.
When a Flat Fee Can Be the Right Fit
It's important to be straightforward here: a flat fee isn't always the wrong choice. There are specific situations where it can make sense.
Low-Volume or Primarily Cash-Based Practices
If your practice is mostly cash-based with only a small number of insurance claims each month, the overhead of a percentage model may not be proportionate. When you're processing fewer than 100 insurance claims monthly and most of your revenue comes directly from patients, a flat-fee arrangement for the limited insurance work can be a practical fit.
Practices with Very Simple Payer Mixes
Some practices have highly consistent visit types, a narrow set of payers, and denial rates that stay below 3% year over year. In those situations, there may be less room for a percentage-based partner to improve on what's already working well.
That said, it's worth verifying this with real data. What looks like a low denial rate sometimes reflects claims that were written off rather than appealed, or visits that were undercoded. A brief audit can confirm whether the numbers are as clean as they appear.
Transitional Periods
Some practices use a flat fee temporarily during a billing transition—such as switching EHR platforms or billing companies—to maintain predictable costs while the new system stabilizes.
This is reasonable, as long as there's a clear timeline for moving into a model that ties billing performance to compensation.
| Practice Characteristic | May Fit Flat Fee | May Fit Percentage-Based |
|---|---|---|
| Claim Volume | Under 100 claims/month | Over 200 claims/month |
| Primary Revenue Source | Cash pay | Cash pay |
| Denial Rate | Consistently under 3% | 5% or higher |
| Growth Plans | Maintaining current size | Scaling or adding providers |
| AR Health | Under 30 days, minimal aging | Over 45 days or growing |
Frequently Asked Questions
Is a 7% billing fee too high for a chiropractic practice?
Not necessarily. A 7% fee under a percentage model means your billing partner earns more only when you earn more. When you factor in the industry-average cost to collect of 3–8% and the administrative rework costs that come with unresolved denials, a percentage fee paired with strong collection results often delivers better net revenue than a lower flat fee.
The clearer question to ask is: what's the total cost of my current billing arrangement, including the staff time my team spends on billing-related tasks?
Do flat-fee billing companies handle appeals and denials?
Some do, and some handle them quite well. But the incentive structure doesn't naturally reward the time-intensive work of complex appeals.
Under a flat-fee model, the billing company's monthly revenue stays the same whether they recover a denied $45 claim or move on. Many flat-fee arrangements cover basic resubmission but may not include multi-level appeals, payer calls, or the follow-through that tends to recover the most revenue.
It's worth reading the contract closely to understand what level of denial management is included.
What is the average cost to collect in healthcare RCM?
Industry benchmarks place the cost to collect between 3% and 8% of net patient revenue, depending on practice size, specialty, payer mix, and billing approach.
Practices with systematic RCM processes and professional billing partners typically fall at the lower end. Those handling billing in-house or using arrangements without clear performance accountability can exceed 10% when you include staff time, software costs, and administrative overhead.
Why do percentage-based billing companies tend to have lower denial rates?
Because every denied claim reduces their income directly.
A percentage-based billing company that allows denial rates to drift upward is effectively lowering its own compensation. That built-in accountability tends to drive consistent behaviors: thorough pre-submission review, proactive payer follow-up, and investment in the training and tools that help prevent denials before they happen.
The structure rewards prevention, not just processing.
Can I switch from a flat fee to a percentage model without disrupting my cash flow?
Yes, and with a clear plan, the transition can be smooth.
A reliable billing partner will start with a practice audit, reviewing your current AR, denial patterns, and payer mix before anything changes. The transition typically takes 30–60 days, with some overlap between systems.
Most practices see improved cash flow within the first full billing cycle under a percentage model. The new partner has a financial reason to address aging AR quickly—every recovered dollar adds to their revenue too.
How does a flat-fee model affect my office manager's workload?
This is one of the less obvious effects, and it's worth considering carefully.
Flat-fee billing arrangements sometimes cover claim submission but leave denial follow-up, patient billing questions, EOB reconciliation, and AR management to the clinic. That work has to go somewhere, and it usually lands on your office manager.
A percentage-based partner typically handles the full revenue cycle because each resolved claim contributes to their income. That broader scope can meaningfully reduce the billing-related workload your team carries.
What should I look for when comparing billing company fee structures?
Start by looking past the headline number.
Ask what services are included versus billed separately. Find out whether appeals, credentialing, and patient billing are part of the standard fee or add-ons. Understand the communication cadence—weekly reporting and proactive updates should be standard.
And make sure the company has specific experience in your practice type. Chiropractic, physical therapy, and allied health billing each have their own nuances, and a billing partner with deep experience in your area will typically deliver better results than a generalist, regardless of fee structure.
Choosing the Right Model for Your Practice
Choosing a billing model is really a decision about what kind of working relationship you want with the company managing your revenue cycle.
A flat fee provides a predictable cost. A percentage model provides shared accountability.
In 2026, with denial rates gradually rising, Medicare reimbursement adjusting, and payer processes becoming more complex, shared accountability tends to produce better outcomes. It creates a sustainable, long-term reason for your billing partner to follow through on every claim—not because they're told to, but because the structure supports it.
The right billing partner brings clarity to your revenue cycle. They keep you informed with transparent reporting, handle the detail work systematically, and treat your practice's revenue as something worth protecting—because it is.
Deciding on a billing model is one of those things that looks simple on the surface but gets more nuanced the deeper you go. If you've made it this far, you're clearly thinking through this carefully.
If you're thinking "this all makes sense, but I don't have time to figure it out," you're not alone. Most clinic owners we work with felt the same way before they realized how much revenue was slipping through the cracks.
That's why we offer a free discovery call. It's a chance to talk through your current billing situation and get clarity on what's working, what's not, and what your options are.
We'll help you understand:
- Where your claims might be getting stuck
- What's causing denials or delays
- Whether your AR is healthy or needs attention
- How your current process compares to best practices
- What a partnership with Bushido would actually look like
Book a Call — no pressure, no obligation, just a straightforward conversation about your billing.
Because every month spent under a billing model that doesn't support your goals is another month of revenue that could be working harder for your practice.
© 2026 Bushido Billing. All Rights Reserved | Web Design by iTech Valet


